| Acute bacterial sialadenitis Acute purulent parotitis Acute postoperative parotitis Acute bacterial submandibular sialadenitis |
| Chronic bacterial sialadenitis Chronic recurrent parotitis Chronic sclerosing sialadenitis of submandibular gland Obstructive sialadenitis |
| Viral sialadenitis Parotitis epidemica (mumps) Cytomegalovirus infection (salivary gland viral disease) Other types (Coxsackievirus, infectious mononucleosis, measles, encephalomyocarditis virus, ECHO virus) |
| Granulomatous sialadenitis Giant cell sialadenitis Tuberculosis |
Acute bacterial sialadenitis
Acute bacterial (suppurative) sialadenitis affects predominantly the parotid and submandibular glands. Sialadenitis of the intraoral and sublingual glands is rare. Primary acute bacterial parotitis (ABP) has been reported mainly in elderly, postoperative patients who are intubated or suffering from dehydration, malnutrition, Sjogren’s disease, poor oral hygiene or recent intensive teeth cleaning, ductal obstructions due to sialolithiasis, tumor or foreign bodies, chronic tonsillitis, dental infection, neoplasm of the oral cavity, liver cirrhosis, or diabetes mellitus. The use of antisialanogic drugs, including antidepressants, anticholinergics, and diuretics, has been associated with acute bacterial sialadenitis. Bacteria can infect the parotid gland by ascending transmission through Stensen’s duct or through bacteremia. Acute postoperative parotitis, as a special type of acute purulent parotitis, is observed particularly after major abdominal surgery and is accompanied by large fluid loss and reduction of salivary secretions. Additional risks include fine-needle aspiration of the parotid and intravascular iodinated radiocontrast agents, especially in older males.
Neonatal suppurative sialadenitis is uncommon. Risk factors include prematurity, decreased saliva production related to prolonged orogastric or nasogastric feeds, dehydration, sialolith, and abnormalities of Wharton’s duct.
The most common pathogens associated with acute bacterial infection are Staphylococcus aureus and anaerobic bacteria, followed by group A strep, Strep viridans, and strict anaerobes, such as Fusobacterium nucleatum, Prevotella, and Porphyromonas. Peptostreptococcus anaerobius may also play a major role. Brook reported 43% of patients with anaerobic infection and 57% with mixed aerobes/anaerobes etiology. Recent reports suggest increasing incidence of gram-negative rods. Less frequently isolated organisms included Arachnia, Haemophilus influenzae, Klebsiella pneumoniae, Salmonella spp., Pseudomonas aeruginosa, Treponema pallidum, cat scratch bacillus, Eikenella corrodens, Actinomyces israelii, and Actinomyces eriksonii.
Patients present with sudden onset of firm, erythematous swelling of the pre- and post-auricular areas that extends to the angle of the mandible, with intense pain and tenderness, trismus, and dysphagia. Fever and chills are common.
Pus can be expressed from the orifice of the Stensen’s duct in 50% of cases (Figure 9.1).
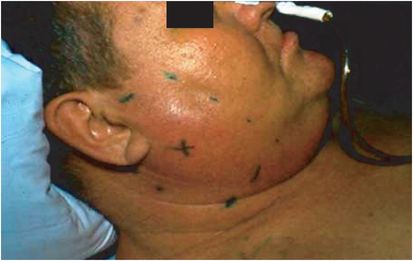
Figure 9.1 Staphylococcal parotitis in a postoperative patient. The enlarged parotid is outlined by ink marks with an X in the center. Note the characteristic diffuse enlargement of the gland, earlobe elevation, and obliterated mandible landmarks. (Courtesy of David Schlossberg, MD.)
Leukocytosis with left shift, elevated sedimentation rate, and increased serum amylase level are frequent.
If purulent discharge is present, it should be Gram stained and cultured, with care to avoid contamination with oral flora. Ultrasound confirms presence of a mass with high sensitivity and can localize disease to the parotid gland. In addition, ultrasound can identify those entities that may not need surgical intervention and can detect stones and differentiate between obstructive and nonobstructive sialoadenitis.
Sialography cannot be used during acute infection and requires the injection of a contrast material. Magnetic resonance sialography is promising. The differential diagnosis of an enlarged parotid mass includes viral parotitis, cystic fibrosis, collagen vascular diseases, alcoholism, chronic recurrent parotitis, sarcoidosis, sialolithiasis, and neoplasms.
Treatment of ABP requires elimination of the cause, e.g., mucus plug, by using adequate hydration to increase the salivary flow, and intravenous systemic antibiotics that cover gram-positive cocci, spirochetes, and mouth anaerobes. Immunocompromised patients with neutropenia or neutrophil dysfunction should have additional coverage for Enterobacteriaceae and pseudomonas pending results of cultures. In cases involving abscess, incision and drainage are performed by surgical exposure of the gland and blunt probing. Antistaphylococcal agents (to also cover methicillin-resistant S. aureus [MRSA]) plus either metronidazole or clindamycin is adequate empiric treatment in immunocompetent hosts. In immunocompromised patients, vancomycin or linezolid can be used in addition to imipenem, meropenem, or piperacillin–tazobactam (Table 9.2). Antibiotics should be given for 10 to 14 days.
| Antibiotic treatment | Surgical treatment | |
|---|---|---|
| Acute bacterial sialadenitis | Susceptible Gm+ : penicillinase-resistant penicillin or first-generation cephalosporin Resistant Gm+ (MRSA, S. pneumoniae): vancomycin Gm− : third-generation cephalosporin, quinolone Anaerobes: flagyl or clindamycin | Parotid drainage may be needed; silolithectomy in submandibular infection |
| Chronic bacterial sialadenitis | Same as above | Gland extirpation usually required |
| Viral sialadenitis | None; symptomatic treatment | None |
| Granulomatous sialadenitis | Director to specific cause | Rarely needed |
Abbreviations: Gm+ gram positive; Gm− gram negative; MRSA methicillin-resistant Staphylococcus aureus.
Adjuvant treatment includes optimal oral hygiene, nutritional support, warm compress, discontinuation of anticholinergic drugs that reduce salivary flow or increase the viscosity of the saliva, and use of sialagogic agents such as lemon juice. Irradiation of the glands is no longer recommended. Needle aspiration of the gland should be avoided. Surgical intervention is indicated for lack of improvement after 3 to 5 days of antibiotic therapy, facial nerve involvement, and abscess formation.
A follow-up CT scan or sialogram is recommended after the resolution of the infection to treat the underlying disease such as calculi or stricture to prevent recurrence. Acute bacterial submandibular sialadenitis (ABSS), unlike ABP, is frequently associated with ductal obstruction by stones or structures. Medical treatment is the same as for ABP. If ductal calculi are present, excision is necessary. Repeated ductal stone formation may cause chronic submandibular infection, in which case surgical excision of the gland is indicated.
Subacute necrotizing sialadenitis (SANS) is an uncommon self-limiting inflammatory disease of unknown origin that has a male to female ratio of 3:1 and an age range from 15 to 70 years old. It usually affects the palatal salivary glands. Patients present with pain and/or swelling. The cause is infarction of the gland from surgery or trauma.
Chronic bacterial sialadenitis
Chronic bacterial sialadenitis (recurrent bacterial sialadenitis) involves parotid or submandibular glands and may follow a subclinical course. It occurs via the excretory duct. Inflammation of the oral mucosa and decreased salivary flow cause ascending infection in the major salivary glands. This chronic infection is sometimes associated with Sjogren’s disease, with associated xerostomia and systemic autoimmune disease. Chronic juvenile recurrent parotitis is a combination of a congenital malformation of a portion of the salivary ducts and infections ascending from the mouth following dehydration. Boys are more often affected than girls. The clinical course includes recurrent episodes of acute sialadenitis of either parotid or submandibular glands. Although the inflammation may occur bilaterally, painful swelling is often
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree





