Abstract
The genetic basis for several of the familial hyperparathyroid syndromes has been identified, and in these instances, genetic testing can make important (and at times lifesaving) contributions to patient/family management. This chapter focuses on the following familial hyperparathyroid syndromes: hyperparathyroidism-jaw-tumor syndrome (HPT-JT), resulting from mutation of the HRPT2 (CDC73) gene; familial hypocalciuric hypercalcemia (FHH), caused by mutation of CASR, GNA11, or AP2S1; neonatal severe hyperparathyroidism (NSHPT) caused by mutation of CASR; and familial isolated hyperparathyroidism (FIHP), which is genetically heterogeneous. Two other important hyperparathyroid syndromes, multiple endocrine neoplasia (MEN) types 1 and 2, are the subjects of separate chapters.
Keywords
parathyroid, hyperparathyroidism, hyperparathyroidism-jaw-tumor syndrome (HPT-JT), HRPT2, CDC73, familial hypocalciuric hypercalcemia (FHH), CASR, MEN1, MEN2, RET, GNA11 , AP2S1
Introduction
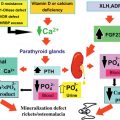
The parathyroid glands function to maintain calcium homeostasis through secretion of parathyroid hormone (PTH). Parathyroid cells express on their surface a G-protein coupled calcium-sensing receptor, CaSR, which has the ability to detect minute deviations in the extracellular concentration of ionized calcium and trigger a corrective response in the amount of PTH released. For example, in defending against a lowering of serum calcium, PTH secretion is increased, and the hormone acts in concert on multiple target organs to increase serum calcium. PTH increases bone turnover including resorption, releasing calcium into the circulation. PTH acts on the kidney to increase tubular reabsorption of calcium, and to increase phosphate loss. PTH also increases the activity of renal alpha-1-hydroxylase, which hydroxylates 25-OH-vitamin D to form 1-25-(OH) 2 -vitamin D, the active form of the vitamin. Active vitamin D induces increased calcium uptake in the intestine, and acts in a feedback loop with the parathyroid glands to decrease PTH synthesis and secretion.
In primary hyperparathyroidism, PTH secretion is increased and is no longer appropriately regulated by ambient calcium levels, resulting in hypercalcemia. Patients with this disorder may suffer from symptoms of hypercalcemia and may manifest consequences of excessive PTH action including bone pain, increased bone resorption, osteopenia, fractures, hypercalciuria, and nephrolithiasis. However, in the United States and other parts of the world where serum calcium measurement is part of routine laboratory screening, the diagnosis is often made in individuals who have few symptoms or are asymptomatic.
Primary hyperparathyroidism is typically caused by abnormal proliferation of one or more parathyroid glands. A solitary benign parathyroid adenoma is the most common pathologic basis for the biochemical diagnosis (85%), and less frequently multigland disease, that is, primary parathyroid hyperplasia, is found (10–20%). More rarely, primary hyperparathyroidism is attributed to other causes such as parathyroid carcinoma (1%) or ectopic secretion of PTH from nonparathyroid tumors.
Generally speaking, the large majority of patients with sporadic primary hyperparathyroidism are not known to carry a strong genetic predisposition, and with the exception of sporadic parathyroid carcinoma, genetic diagnosis has no current role in this setting. That said, the discovery that some patients with sporadic parathyroid adenomas have rare germline variants in cyclin-dependent kinase inhibitor genes suggests that such variants, despite their apparently insufficient penetrance to yield clear familial clustering, may importantly contribute to sporadically presenting hyperparathyroidism. Further study of these patients and variants, plus others to be discovered, could ultimately define a clinical role for specific genetic information as an example of “personalized medicine.” Familial hyperparathyroidism is rare in comparison to sporadic disease; less than 10% of primary hyperparathyroidism is linked to heritable genetic causes. However, the genetic basis for several of these familial syndromes has been identified, and in these instances genetic testing can make important (and at times life-saving) contributions to patient/family management. In this chapter, we will focus on the following familial hyperparathyroid syndromes: hyperparathyroidism-jaw tumor syndrome (HPT-JT), familial hypocalciuric hypercalcemia (FHH), neonatal severe hyperparathyroidism (NSHPT), and familial isolated hyperparathyroidism (FIHP). Two other important hyperparathyroid syndromes, multiple endocrine neoplasia (MEN) types 1 and 2, are the subjects of separate chapters. A summary of hyperparathyroid disorders and the genes known to be involved, either through acquired or germline mutation, is provided in Table 11.1 .
| Parathyroid disorder | Gene(s) involved * |
|---|---|
| Sporadic parathyroid adenoma | Cyclin D1 (somatic); MEN1 (somatic); CDKN1B and other CDKIs (somatic and germline) |
| Sporadic parathyroid carcinoma | HRPT2 / CDC73 (somatic and germline) |
| MEN1 (or MEN4) | MEN1 ; CDKN1B (in MEN4 ); and other CDKIs |
| MEN2 | RET |
| HPT-JT | HRPT2/CDC73 |
| Familial hypocalciuric hypercalcemia (FHH) | CASR ; GNA11 ; AP2S1 |
| Neonatal severe hyperparathyroidism (NSHPT) | CASR |
| Familial isolated hyperparathyroidism (FIHP) | MEN1 ; HRPT2 ; CASR ; other gene(s), unidentified |
Hyperparathyroidism-jaw tumor syndrome (HPT-JT), HRPT2 , and parathyroid carcinoma
Introduction
Hyperparathyroidism-jaw tumor syndrome (HPT-JT) is an autosomal dominant condition that results from mutation of the HRPT2 ( CDC73 ) tumor suppressor gene. HPT-JT includes a predisposition to parathyroid tumors, ossifying fibromas of the jaw, renal lesions such as bilateral cysts, hamartomas, or Wilms’ tumors and uterine adenomas. Hyperparathyroidism occurs with about 80% penetrance in HPT-JT. All parathyroid cells are at risk for tumor development over the individual’s lifespan, and tumors might arise in multiple glands simultaneously, or asynchronously in one gland at a time over many years. Other distinctive features of the hyperparathyroidism in carriers of HRPT2 germline mutations include a tendency to develop cystic parathyroid adenomas and, importantly, a markedly increased risk of parathyroid carcinoma (10–20%).
Parathyroid carcinoma can be difficult to distinguish from benign adenoma on purely histological grounds, and its unequivocal diagnosis requires the presence of local invasion into surrounding tissues and/or distant metastasis. Histologic features frequently present in parathyroid carcinoma, but insufficient for its diagnosis, include cytologic atypia, nuclear pleomorphism, capsular invasion, fibrous bands, and mitoses. Early surgical treatment by en bloc resection is necessary to cure parathyroid carcinoma, since metastatic disease is very difficult to control and usually results in death from hypercalcemia and metabolic complications. As described in the subsequent section, the association of parathyroid carcinoma with HPT-JT also led to the discovery of the role of HRPT2 mutation in sporadic parathyroid carcinoma.
Genetic Pathophysiology
The HRPT2 gene, located on chromosome region 1q25-q32, encodes a 531 amino acid nuclear protein termed parafibromin. A nuclear localization signal resides at amino acids 136–139. Human parafibromin has homology to the yeast cdc73 protein and has been shown to have an analogous function, interacting with Paf1, Leo1, Ctr9, and RNA polymerase II in the Paf1 complex to play a role in transcript elongation and 3′ end processing. Parafibromin downregulation promotes the S phase of the cell cycle, consistent with its role as a tumor suppressor gene. Despite these insights, precisely how the loss of parafibromin function leads to parathyroid cell transformation and the other manifestations of HPT-JT remains to be understood.
Most germline mutations in HPT-JT kindreds are predicted to inactivate or eliminate parafibromin, and examples of inactivating somatic mutations in the remaining allele were found in HPT-JT-associated tumors. This pattern of biallelic inactivating mutation suggested a classical tumor suppressor function for HRPT2 , consistent with Knudson’s two-hit model. HRPT2 mutations have been detected in about 70% of kindreds with HPT-JT, typical of a tumor suppressor syndrome, the assumption being that most, if not all, of the remaining families have mutations in the same gene but escape detection because the usual sequencing strategy is limited to the coding exons. No HPT-JT families are known to show linkage to loci other than the 1q region in which HRPT2 lies. In addition, again typical for a tumor suppressor and reflecting the numerous ways in which a gene can become inactivated, mutations are dispersed throughout HRPT2 without any highly specific hot spot.
The familial predilection to parathyroid carcinoma in HPT-JT led to investigation of the hypothesis that acquired (somatic) mutation of the HRPT2 gene might participate in the pathogenesis of sporadic, nonfamilial parathyroid carcinomas. Not only were somatic HRPT2 gene mutations found in sporadic carcinomas, indicating that they confer a strong selective advantage leading to parathyroid cell malignancy, but these mutations were detected with an impressively high frequency of 75%. Again, because many tumors would be expected to have HRPT2 gene mutations that would have been missed with the current sequencing strategies, it is likely that virtually all parathyroid carcinomas are driven by HRPT2 mutation.
Importantly, a subset of patients with apparently sporadic parathyroid carcinoma were unexpectedly found to harbor germline, heritable mutations in the HRPT2 gene. Such patients may have de novo mutations or otherwise represent newly discovered but phenotypically classical HPT-JT, or they may represent a distinct phenotypic variant with unknown penetrance of parathyroid carcinoma. This discovery that relatives of patients with apparently sporadic parathyroid carcinoma can themselves be at risk for parathyroid malignancy by inheriting an HRPT2 gene mutation provided a new indication for genetic testing.
Diagnosis Genetic Testing and Interpretation
Direct sequencing of the full coding region of the HRPT2 gene is the standard approach to DNA mutational testing. Typical for a tumor suppressor gene, there is no focused hot spot for detectable mutations within the gene, and therefore the entire gene must be analyzed when the mutation is not already known. As noted earlier, a negative result in a potential proband is not conclusive, given that even among typical HPT-JT kindreds, a false negative rate of about 30% exists. Thus, in the setting of a negative DNA sequencing result, a search for relevant phenotypic traits (e.g., using jaw imaging, renal ultrasound) can be especially valuable, and appropriate surveillance for development of hyperparathyroidism should receive consideration taking pretest likelihood into account. A negative test result provides more valuable information in an asymptomatic relative in a family with a known mutation, since the absence of that specific mutation would indicate that the individual did not inherit the predisposing allele. A list of resources and laboratories that perform HRPT2/CDC73 DNA testing is available at www.genetests.org or www.ncbi.nlm.nih.gov/gtr .
HRPT2 gene sequencing can be considered in probands with known or suspected familial HPT-JT or familial isolated hyperparathyroidism, as well as patients who present with apparently sporadic carcinoma. Testing of the latter is indicated in most instances because of the known presence of otherwise unsuspected germline mutations in a substantial minority of these individuals. Knowledge that an individual bears a germline mutation of HRPT2 has important implications. In a phenotypically classical HPT-JT kindred, identification of the proband’s mutation enables family members to be easily and less expensively genotyped for the presence or absence of that specific mutation, since only that region must be sequenced to determine if the diseased allele was inherited. Asymptomatic relatives found not to carry the mutation can be spared ongoing surveillance for parathyroid malignancy. Asymptomatic, normocalcemic relatives who do carry the mutation can be monitored in a surveillance program that includes regular testing for the development of biochemical primary hyperparathyroidism, directing early surgical treatment to cure or prevent malignant parathyroid neoplasia. Similar considerations apply in the situation of suspected or clear familial isolated hyperparathyroidism in which an HRPT2 gene mutation is uncovered, or in relatives of mutation-positive patients with sporadic parathyroid carcinoma. Additionally, in the latter two settings, treatment of a proband already affected with hyperparathyroidism can be altered by a positive genotype as described in the subsequent section, related to the recognition that all parathyroid tissue in such individuals remains at increased risk for new tumor development.
Prenatal or preimplantation testing is possible in the setting of a known familial HRPT2 gene mutation. However, issues related to this possibility – including the likelihood that mortality from parathyroid cancer in mutation carriers could be largely eliminated by surveillance and early surgery – would need to be factored into these considerations. There are no reports of such testing to date, and its use appears to be rare.
Another potential role for HRPT2 DNA testing would be in the diagnosis of parathyroid carcinoma, particularly in sporadic presentations. In this instance the idea would be to examine parathyroid tumor tissue for somatic mutations, which are highly specific to parathyroid cancer as opposed to sporadic benign adenomas. In practical terms, the value of such testing would likely be primarily for so-called “atypical parathyroid adenomas,” which are diagnostically equivocal, containing some cancer-associated features while failing to meet the strict criteria for diagnosis of carcinoma. This possibility requires further study before its clinical utility can be said to be established. Similarly, studies have been directed at using immunohistochemical assessment of parafibromin expression as a surrogate marker for HRPT2 gene mutation, for the same diagnostic purpose. Again, the clinical utility of this approach remains under investigation.
Treatment
A positive test, which uncovers a germline mutation in the HRPT2 gene in a normocalcemic, phenotypically unaffected member of an HPT-JT or FIHP kindred, or relative of a patient with sporadic parathyroid carcinoma, would indicate the need for steps to prevent mortality from parathyroid carcinoma. The best ways to accomplish this are under discussion, but most would agree with a recommendation of careful surveillance by monitoring PTH and calcium levels every 6–12 months. It should be emphasized that in the interpretation of such surveillance testing, a low threshold should be maintained for acting upon biochemical results that suggest the development of primary hyperparathyroidism and a low threshold for moving to parathyroid surgery if such results are confirmed. The reported presence of biochemically nonfunctional parathyroid carcinoma in a family with an HRPT2 gene mutation has led to consideration of whether diagnostic imaging studies should also be part of a surveillance program.
Surgical treatment must be thorough, given the malignant potential of parathyroid neoplasms in individuals with HRPT2 germline mutation, the fact that all parathyroid tissue is at risk, and that initial complete resection offers the best chance to prevent mortality from metastatic disease. However, the approach should also take into account that most parathyroid tumors in HPT-JT are benign. Therefore, the recommended approach to parathyroid surgery in HRPT2 gene mutation-positive patients is quite different from that often taken for typical sporadic hyperparathyroidism. For the latter group, in which a solitary benign adenoma is the most common finding, a focused minimally invasive parathyroidectomy is often used. In contrast, mutation-positive patients should have a bilateral neck exploration, with the goal of identifying all parathyroid glands. Any gland that appears abnormal should be removed en bloc . Whether to also resect normal-appearing glands, which all carry the genetic potential to give rise to parathyroid cancers in the future, has been the subject of some discussion. At this time, we favor leaving the normal glands in situ , possibly tagging them to facilitate identification in a subsequent operation. This suggestion is influenced by: (1) the well-known difficulties faced by patients contending with currently available lifelong replacement therapy for hypoparathyroidism; (2) the fact that the majority of mutation-positive individuals would not be expected to ever develop metastatic parathyroid disease; and (3) the likelihood (still to be proven) that an ongoing program of careful surveillance and, when needed, repeat surgery, would continue to identify tumors early enough to effectively prevent death from parathyroid malignancy. As discussed earlier, a negative DNA mutation result in a proband does not rule out the condition, so the same approach to surveillance and surgery can be appropriate when there is sufficient clinical suspicion of an HRPT2 gene mutation, even if a mutation was not detected or if DNA testing was not performed.
Genetic counseling for those with HRPT2 gene mutations should focus on the potential for malignant parathyroid carcinoma, while also reassuring the individual that benign adenoma is the more common pathology in HPT-JT. When appropriate, the importance of continued monitoring of serum calcium and PTH levels to diagnose parathyroid disease promptly and minimize the potential for metastatic spread should be emphasized. Involvement of an experienced endocrinologist and endocrine surgeon is strongly advised.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree