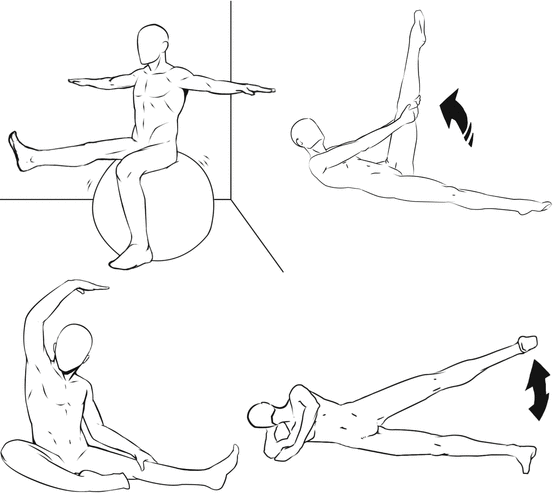
Fig. 9.1
This figure shows the imbalance between the gravity center and the supporting base in older adults
Moreover, flexed posture determines an overload to the lower limbs and to the spine.
Gait also changes during aging, as a consequence of a reduction in muscular capacity, sensory function, and neural processing [13]. Muscle weakness of hip abductors and adductors has been reported, and a greater instability of elderly people when initiating stepping has been reported in elderly people [15]. Older adults tend to slow their walking speed and to show a slower reaction to external stimuli [15–21]. The loss of plantar cutaneous sensation is another important factor leading to impairment of motor control [21].
9.3 Frailty Measurement
Identifying frail older people is the first and essential step in rehabilitation. Multiple scales have been developed, but the most common are the Fried frailty phenotype assessment and the frailty index of accumulative deficits (FI-CD) index. According to Fried’s criteria, frailty is defined by the presence of three or more criteria and pre-frail state by the presence of one or two of the following: shrinking (unintentional weight loss of 4.5 kg or more in the last year), weakness (low grip strength), exhaustion, slowness (slow walking speed), and low physical activity. Fried’s criteria are also predictive of adverse clinical outcomes, including mortality. They are, however, not commonly used for routine assessment and cannot be routinely applied in acutely ill or severely disabled patients; moreover, they do not include the psychosocial components [3].
9.4 Physiotherapy in Frail Older Adult
Frailty is a modifiable dynamic process that can be prevented and even reversed by early identification and treatment of pre-frail older adults. Specific strategies could be therefore be used in order to attain this goal, and the best results seem to be obtained by combining exercise and nutritional supplementation [22].
Scientific literature showed that regular physical activity reduces the risk of developing cardiovascular and metabolic diseases, obesity, cognitive decay, osteoporosis, and muscular atrophy as well as the risk of falls in both healthy and frail elderly people [23]. There is, however, a great variety among the studies concerning the number of patients enrolled, degree of frailty, training programs, and assessments.
Generally, the more a person is physically active, the better will be its physical performances. This is due mainly to a better adjustment in the hemodynamic (a more efficient distribution of oxygen and nutrients to the tissues) and in the motor coordination in response to environmental changes [23–26].
International guidelines highlighted the importance of multimodal interventions that combine strength activities, cardio conditioning workout, and balance and functional exercises. Nevertheless—although the scientific community unanimously promotes regular physical activity of elderly people—participation to exercise programs progressively decreases during aging and, concomitantly, the desire to participate. This is the reason why it is important to define a personalized exercise program, responding to subject’s own features and expectations (taking into account the level of previous physical activity), its social engagement, and the support of caregivers.
Various exercise modalities have been proven to be effective in older patients, but the combination of strength, resistance, power, coordination, proprioception, and balance and aerobic training is the most beneficial.
The effect of exercise on falls was studied in terms of incidence, and risk of falls and fear of falling were studied, but results were controversial.
The exercise has a positive influence on body and muscle composition, is beneficial for mobility, and improves older patients’ functional abilities [27]. Therefore, it is always important, when starting a training program, to find the appropriate level of dosage, intensity, frequency of an exercise, as well as the correct level of progression; physical exercise should always be administered and scheduled according to the goals and the physical fitness of the subject.
9.5 Strength Training and Aerobic Exercise
An exercise program should last 3–4 months in average, with a maximum frequency of 3 sessions/week of at least 45 min each. Every session must include a phase within the aerobic threshold, related to daily life activities, such as walking, cycling, climbing stairs, or recreational activities (exercises with a ball) and a part dedicated to the muscular strengthening, using free weights, elastic resistance, etc.
The exercise intensity is variable, according to the exercise experience and physical fitness of each subject.
Repetition maximum (1RM) is the maximum force that can be developed in one maximal contraction. 1RM test is generally employed to measure the intensity of an exercise. There is not a common agreement in the literature, on the amount of intensity to be adopted during an exercise; however, the majority of authors suggest that the intensity should be light or moderate (20–30% 1RM) and slowly increased progressively (i.e., it can be obtained by increasing the percentage of 1RM up to a maximum of 80% 1RM or the number of repetitions from 8 to 15 repetitions for one series). An increase in exercise intensity is allowed no more than once every 4 weeks, or when the series is perceived as easy to perform. Currently, there is no evidence on the muscular groups to train; several recent studies focused their attention on the plantar flexors, since a loss of strength in this group is associated with a reduction of walking speed while an increase to an improvement in balance. No risk in executing muscular strength training has been shown; however, some minor musculoskeletal symptoms have been reported (e.g., diffuse arthralgia, joint and muscle swelling, fatigue, or even muscular sprain, especially in those subjects who started from very debilitated or sedentary conditions) (Figs. 9.2 and 9.3).
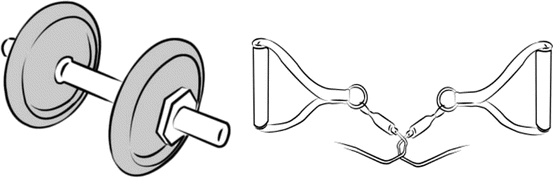
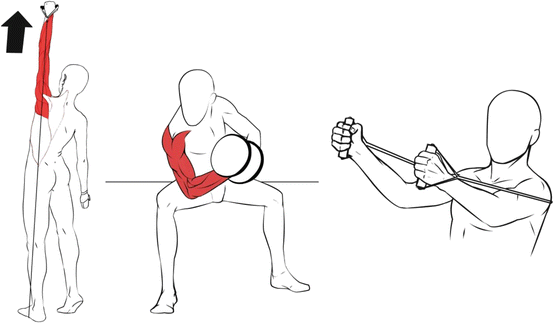

Fig. 9.2
This figure shows some tools that are commonly used for strength and power training. Dumbbells, a type of free weight, can be used for reinforcement of the upper limbs. Elastic bands and elastic tubes can be used for strength training of both upper and lower limbs

Fig. 9.3
Examples of exercises using dumbbells and elastic bands
The risk of serious adverse events after cardiopulmonary training is low for both moderate and elevated efforts, and it is higher during the first weeks of training. This training determines central and peripheral circulatory adjustments and aims to increase the musculoskeletal system’s ability to produce energy through the oxidative pathways. The first week cardiopulmonary training should start from 5 to 10 min of activity per session and then progressively increase up to 15–30 min.
The methods for controlling training intensity are different. The most frequently employed are the heart rate, which should be kept between 70% and 80% of the maximum heart rate (HRmax) in order to maintain oxidative metabolism, or self-monitoring scales, which evaluate the perceived fatigue, in which the intensity should be between moderate and well tolerated (12–14 on the 20 point Borg scale) (Figs. 9.4, 9.5, and 9.6).
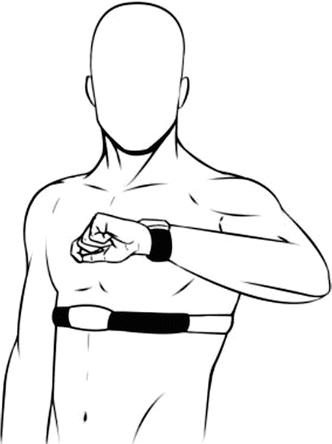
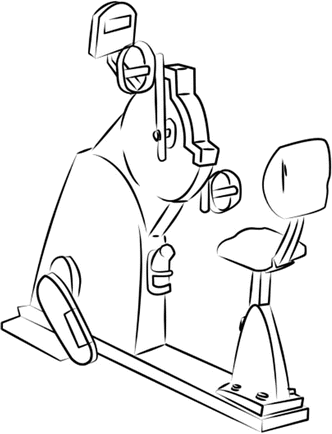
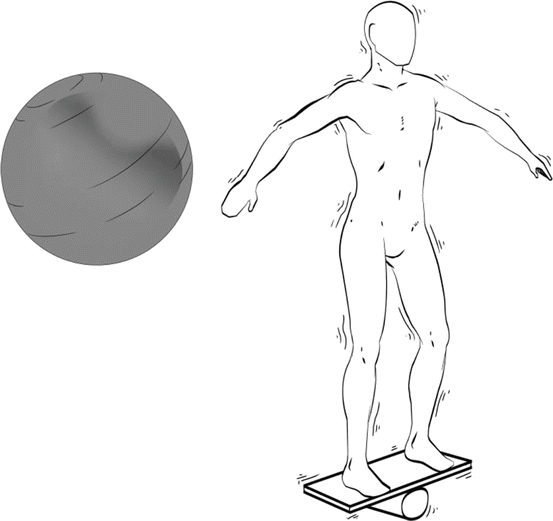

Fig. 9.4
Cardiopulmonary training. Watch or chest strap are simple, wearable tools used to monitor heart rate and the intensity during exercises

Fig. 9.5
The ergometer is a machine used for cardiopulmonary training that allows measuring the work performed by exercising

Fig. 9.6
Unstable surfaces (balance pillows, boards, or balls) are commonly used to improve balance and postural control
9.6 Balance
Balance exercises are mainly functional and progressively difficult, allowing the body to develop anticipatory abilities, in relation to different tasks or environmental situations.
In order to improve their balance, subjects must exercise themselves against an external force consequent to their movements or applied from outside.
Examples of exercise interventions are walking and tandem walking, cycling, proprioceptive static and dynamic exercises (e.g., using balance balls), strength exercises, and computerized balance training with visual feedback, coordination exercises, dance, tai chi, and yoga. Exercises can be proposed either singularly or combined. Different tools are used to improve balance and postural control such as proprioceptive or unstable surfaces and systems using computerized visual or acoustic feedback (Fig. 9.6).
Duration of the exercises ranges from a minimum of 4 weeks to a maximum of 12 months, with sessions taking place from twice a week up to once a day. The most common frequency is three times a week. Duration of the single session varies from 3 to 90 min, with a major frequency of 60 min.
Stretching and coordination exercises can also be useful in older patients. Coordination exercises aim to prepare older patients in managing external disturbing forces and allow a better control of the center of gravity during walking, thus reducing the risk of falls (Figs. 9.7 and 9.8) [28].