Breast cancer is the most commonly diagnosed cancer among women. Recent improvements in healthcare, including earlier detection and effective treatment strategies, have significantly improved survival rates. With more than 3.8 million breast cancer survivors in the United States, the 5-year survival rate is 90% and the 10-year survival rate is 80%. Therefore, most patients diagnosed with breast cancer will become long-term survivors. Breast cancer predominantly affects women, with less than 1% of all breast cancers occurring in men, thus much of the information on breast cancer survivorship is geared toward women. Breast cancer survivors frequently experience a number of physical and psychosocial issues that can affect their health and wellbeing. Cancer programs and clinicians need to be prepared to address these long-term effects of cancer and its treatment. The term “cancer survivor” most commonly refers to any person who has been diagnosed with cancer, but the needs of patients with metastatic disease are different from those with curative intent disease. This chapter will review and discuss the essential elements of survivorship care in community oncology practice for breast cancer patients diagnosed with curative intent disease.
Surveillance
The primary goals of surveillance are to watch for recurrence of the original cancer or development of a second cancer. Patients with early-stage breast cancers (tumor <5 cm and fewer than four positive nodes) may follow up with their primary care provider 1 year after their diagnosis, according to the American Society of Clinical Oncology. Crabtree et al. found that there are differing views regarding primary care’s role in cancer survivorship care that includes a “lack of coherence” about the overall concept of survivorship. The authors found that in spite of a growing number of cancer survivors in the United States as well as a shortage of oncologists, some primary care providers believe that care after cancer treatment has ended should continue to be done by the oncology team. Table 13.1 summarizes current surveillance recommendations for breast cancer survivors, as outlined in this section.
| Mode of Surveillance | Recommendation |
|---|---|
| History/physical examination | Every 3–6 months for the first 3 years after primary therapy, then every 6–12 months for the next 2 years, and then annually |
| Mammography | Mammography should be performed yearly |
| Pelvic examination | Regular gynecologic follow-up is recommended for all women. Patients who receive tamoxifen therapy are at increased risk for developing endometrial cancer and should be advised to report any vaginal bleeding to their physicians. Longer follow-up intervals may be appropriate for women who have had a total hysterectomy and oophorectomy |
| Bone density testing | Those at risk for developing bone loss due to medication should be screened with a bone density test every 2 years |
Regular assessment with history and physical examination, including a clinical breast examination, remains the mainstay of detecting breast cancer recurrence. The physical examination should be performed by a clinician who is experienced in doing breast examinations and should include examination of the affected breast, if present, as well as the chest wall, the contralateral side, bilateral axillary regions, and the supraclavicular fossas. If lymphedema is present, circumferential measurement of both upper extremities should be done. It is also recommended that palpation of the spine, sternum, ribs, and pelvis for bone tenderness should be routinely performed. Cardiac evaluation, as well as assessment of the lungs and abdomen, and a neurologic assessment that evaluates balance, gait, and sensory and motor function are important as well. Routine gynecologic follow-up is recommended for women who have not undergone total hysterectomy, particularly patients who are prescribed tamoxifen, as they are at increased risk for developing endometrial cancer. Follow-up recommendations for breast cancer survivors are summarized in Table 13.1 .
Imaging
Mammography
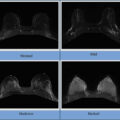
Mammography continues to be the imaging standard for breast cancer screening. The use of digital breast tomosynthesis as opposed to full-field digital mammography reduces recall rate and improves sensitivity and specificity. Variability exists in guideline recommendations for surveillance initiation, interval, and cessation. According to the National Comprehensive Cancer Network (NCCN), American Cancer Society, and American Society of Clinical Oncology (ASCO), annual mammograms are recommended for women who have had breast-conserving surgery (partial mastectomy or lumpectomy) and/or radiation. Women who have had a simple, modified radical or radical mastectomy should continue to have a yearly mammogram on the remaining breast.
Magnetic Resonance Imaging Breast magnetic resonance imaging (MRI) is not routinely recommended for surveillance due to insufficient evidence that it is any better than mammography in detecting breast cancer recurrence. However, it can be a useful diagnostic tool, specifically for women with a known BRCA1 , BRCA2 , or other high-risk genetic mutation and/or those who have a strong family history.
Genetics
If not already done by the time of survivorship, women who are at high risk of familial breast cancer syndromes and all men with breast cancer should be referred for genetic counseling. As an alternative to surveillance, women with a personal history of breast cancer and genetic mutation may want to consider bilateral mastectomy, which can be performed at the time of diagnosis or at a later point. The criteria to recommend referral for genetic counseling includes:
- •
Ashkenazi Jewish heritage.
- •
History of ovarian cancer at any age in the patient or any first- or second-degree relatives.
- •
Any first-degree relative with a history of breast cancer diagnosed before the age of 50 years.
- •
Two or more first- or second-degree relatives diagnosed with breast cancer at any age.
- •
A patient or their relative with a diagnosis of bilateral breast cancer.
- •
History of breast cancer in a male relative.
Breast Cancer Tumor Marker Testing and Other Blood Tests
For routine surveillance, it is not recommended to test with CA 15-3, CA 27.29, and CEA tumor markers. In addition, laboratory studies and other radiologic tests have not been shown to be helpful in breast cancer surveillance in asymptomatic patients.
Bone Density Testing
Women with a history of breast cancer may be at increased risk of developing osteoporosis because of their prior cancer treatment, as well as the use of aromatase inhibitors (AIs) for prevention of recurrence in hormone receptor–positive breast cancer in postmenopausal women. NCCN guidelines recommend that women with breast cancer treated with an AI should have a baseline bone density test and then have periodic scans, although the frequency of long-term screening is not specified. ASCO recommends that cancer survivors at risk for developing bone loss due to medication should be screened with a bone density test every 2 years, or more frequently if deemed medically necessary.
Screening for Secondary Cancers
Screening for secondary malignancies related to diagnosis and treatment after breast cancer is an important part of survivorship. A second breast cancer in the opposite breast, or in the same breast for women who were treated with breast-conserving surgery, is the most common occurrence for these patients. Li et al. found that the cumulative incidence of developing second primary cancers after early-stage initial primary breast cancer was 7.43% at 10 years, 14.41% at 15 years, and 20.08% at 20 years. Radiation therapy was also associated with increased risk of secondary cancers. Hormone status has been found to affect one’s risk of secondary malignancy. Women with hormone-positive disease have a decreased risk of developing a secondary primary breast or ovarian cancer, but they have an increased risk of urinary tract cancers, possibly due to hormone use. Smoking history, obesity, and high blood pressure are also risk factors for the development of second primary cancers, underscoring the need for counseling about healthy lifestyle habits. Aside from physical examination and yearly mammograms, there are no recommended screening tests for secondary cancers. Breast cancer survivors should be educated to watch for the following symptoms:
- •
New lumps in the breast
- •
Changes to the skin of the breast, including inflammation and redness
- •
Nipple discharge
- •
Thickening along or near the mastectomy scar
- •
Swollen lymph nodes
- •
New and unexplained pain, especially chest, back, or hip pain
- •
Persistent cough and/or difficulty breathing
- •
Loss of appetite and/or weight loss without trying
- •
New and/or progressive headaches
- •
New or increased seizure activity
Assessment and Management of Physical and Psychosocial Long-Term and Late Effects of Breast Cancer and Treatment
Body Image
Studies have found that over 50% of all breast cancer patients experience issues with body image. The loss of one or both breasts, weight changes, and hair loss are just a few of the changes that can lead to body image distress and subsequent depression and anxiety. Poor body image perceptions can also negatively impact personal relationships and sexual functioning. The negative impact on self-image and self-esteem can pose a significant challenge for patients and lead to diminished quality of life. In 2021, Morales-Sanchez et al. conducted a systematic review of interventions to improve body image and self-esteem in breast cancer survivors. They identified group therapy and support, physical activity programs, and cosmetic-focused interventions as helpful with alleviating body image distress, to varying degrees of effectiveness.
Lymphedema
Breast cancer lymphedema, defined as a progressive swelling of either the proximal portion or the distal digits of the arm, is a potentially irreversible complication of breast cancer and its treatment. It is caused by the disruption of lymphatic flow after axillary surgery and radiation. A 2013 meta-analysis found an estimated risk of 17% among patients with breast cancer, with risk increasing up to 2 years after surgery. The risk of developing lymphedema is 20% higher in those who undergo a complete axillary lymph node dissection in comparison to those who undergo a sentinel lymph node biopsy, whose risk is approximately 5.6%. Patients should be alert to bring any early signs of infection in the extremity to the attention of their physician for consideration of early use of antibiotics. The American Physical Therapy Association uses the maximum limb girth difference between the affected and unaffected arm to classify lymphedema ( Table 13.2 ).
| Mild lymphedema | Maximum girth difference <3 cm |
| Moderate lymphedema | 3–5-cm difference |
| Severe lymphedema | Difference >5 cm |
Education about exercises to help the lymph fluid drain should be a part of a survivorship visit, especially for those who have undergone lymph node dissection. If needed, counseling about weight loss can also improve symptoms in survivors who develop lymphedema. Referral to physical therapy for manual lymphatic drainage, massage, and compression bandages or sleeves can yield positive results. Compression garments should be fitted by an experienced therapist, and patients should be encouraged to wear them regularly and to replace them every 6 months to maintain proper fit. Daily intermittent compression with a pneumatic compression pump is another treatment option. Complex decongestive therapy is a multimodal regimen consisting of manual lymphatic drainage, compression bandaging, exercises to enhance lymphatic drainage, and skin care. Surgical and ablative procedures such as lymphovenous anastomosis, lymph node transplantation, and liposuction have yielded mixed results and should only be pursued when other treatment options have failed.
Cardiotoxicity
In the general population, cardiovascular disease is the number-one cause of death in women. Breast cancer survivors who are obese, smokers, and/or over the age of 60 years, and those with a history of hypertension, diabetes, and hyperlipidemia, have an increased risk of developing early or delayed heart disease after treatment. Cardiac issues including left ventricular dysfunction, heart failure, valvular disease, and congestive heart disease can develop over time in these patients. Antiestrogen treatment with AIs can lead to the development of hypertension, hyperlipidemia, and ischemic heart disease. Survivors with a history of hormone-positive disease need ongoing surveillance for these comorbidities. Breast cancer survivors should be educated about signs of cardiotoxicity, as well as have a yearly review of systems and physical examination to assess for cardiac complications. Table 13.3 lists the potential cardiotoxic effects of cancer treatment. Women on AIs should have routine lipid assessments and intervention if needed. The Heart Failure Association Cardio-Oncology Study Group has developed some guidelines for risk assessment and ongoing surveillance. In those who received treatment with anthracyclines, measurement of left ventricular ejection fraction (LVEF) is recommended 6–12 months after completion of treatment. For those who received human epidermal growth factor receptor 2–targeted therapies, LVEF plus troponins and B-type natriuretic peptide should be measured every 6 months for up to 2 years after completion of therapy. ASCO has also published guidelines for cardiovascular surveillance in cancer survivors:
- •
Echocardiogram should be performed between 6 and 12 months after completion of cancer-directed therapy in asymptomatic patients considered to be at increased risk of cardiac dysfunction.
- •
Cardiac MRI or multiple-gated acquisition may be offered for surveillance in asymptomatic individuals if an echocardiogram is not available or technically feasible (e.g., poor image quality), with preference given to cardiac MRI.
- •
Cardio-oncology referral for asymptomatic cardiac dysfunction during routine surveillance.
- •
No recommendations can be made regarding the frequency and duration of surveillance in patients at increased risk who are asymptomatic and have no evidence of cardiac dysfunction on their 6–12-month post-treatment echocardiogram.
- •
Clinicians should regularly evaluate and manage cardiovascular risk factors such as smoking, hypertension, diabetes, dyslipidemia, and obesity in patients previously treated with cardiotoxic cancer therapies. A heart-healthy lifestyle, including the role of diet and exercise, should be discussed as part of long-term follow-up care.
| Treatment Modality | Potential Cardiovascular Effects |
|---|---|
| Anthracyclines (doxorubicin, epirubicin): doxorubicin ≥250 mg/m 2 or epirubicin ≥600 mg/m 2 | Left ventricular dysfunction, myocarditis, pericarditis, atrial fibrillation, heart failure |
| Alkylating agents (cyclophosphamide) | Left ventricular dysfunction, heart failure, myocarditis, pericarditis, arterial thrombosis, bradycardia, atrial fibrillation, supraventricular tachycardia |
| Endocrine therapy (aromatase inhibitors, tamoxifen) | Venous thrombosis, thromboembolism peripheral atherosclerosis, dysrhythmia, vascular dysfunction, pericarditis, heart failure |
| HER-2 directed therapies | Left ventricular dysfunction, heart failure |
| Radiation: high-dose radiation therapy when heart is in the field of treatment; radiotherapy ≥30 Gy | Coronary artery disease, cardiomyopathy, valvular disease, pericardial disease, arrhythmias |
Cognitive Impairment
Between 15% and 25% of breast cancer survivors experience cancer-related cognitive impairments after treatment. They typically describe concentration problems and difficulty remembering names and numbers, word finding, or multitasking after treatment. Deficits in verbal and visuospatial abilities, as well as executive functioning and processing speed, are the primary cognitive domains affected. Symptoms are typically mild to moderate and are often short term, although some may experience persistent impairment. It is thought that these cognitive changes are multifactorial and may be impacted by psychological issues such as cancer-related distress, depression, anxiety, and insomnia. Survivors who received higher doses of chemotherapy, are postmenopausal, and/or are over the age of 65 years seem to be particularly vulnerable. Tamoxifen use may also be a contributing factor.
Changes to lifestyle behaviors can often help alleviate symptoms. Survivors should be counseled about optimizing stress management, physical activity, sleep quality, and fostering supportive social relationships. For those who continue to experience significant cognitive dysfunction that negatively impacts their daily activities after 12 months of completing chemotherapy or during hormone therapy, a referral to a neuropsychologist may be warranted. Neuropsychological testing can provide an in-depth assessment of objective cognitive functioning and cognitive rehabilitation can be helpful. A recent meta-analysis found that meditation/mindfulness-based stress reduction, cognitive training, cognitive rehabilitation, and exercise interventions for cognitive dysfunction showed statistical significance in improving symptoms.
NCCN survivorship guidelines state that currently there is no effective brief screening tool to assess cognitive dysfunction in the clinical setting and that existing tools, such as the Mini Mental State Examination (MMSE), do not strongly correlate with patient reports of cognitive dysfunction. NCCN guidelines do provide some self-management strategies for patients, as follows:
- •
Teach enhanced organizational strategies and utilize memory aids such as notebooks and planners, using reminder notes, and smart phone technology.
- •
Encourage patients to do the most cognitively challenging tasks at the time of day when energy levels are highest.
- •
Provide information about relaxation and stress-management skills.
- •
Recommend routine physical activity.
- •
Recommend limiting the use of alcohol and other agents that alter cognition and sleep.
- •
Consider meditation, yoga, mindfulness-based stress reduction, and cognitive training, including puzzles and other brain games.
- •
Optimize management of depression and emotional distress, as well as sleep disturbance.
- •
Validate the experience of cognitive dysfunction associated with cancer diagnosis and treatment, and provide reassurance that this is usually not a progressive neurologic disorder.
Distress, Depression, and Anxiety
Breast cancer patients often suffer from psychological distress, which can compromise their quality of life even after their treatment is completed. Research has shown that anxiety and depression are twice as prevalent in cancer survivors as in the general population. Psychosocial distress and depression should be routinely assessed at survivorship visits. There are a number of tools that are used with cancer patients to screen for distress; Table 13.4 lists some of the tools most often used.
| Screening Tool | Description |
|---|---|
| Personal Health Questionnaire (PHQ-9) | 9-item scale composed of questions that correspond to Diagnostic and Statistical Manual of Mental Disorders (DSM-IV) diagnostic criteria for a major depressive episode |
| Personal Health Questionnaire (PHQ-2) | The PHQ-2 consists of the two main criteria for a major depressive episode, specifically depressed mood and anhedonia within the past 2 weeks |
| Hopkins Symptom Checklist (HSCL) | The 25-item version consists of a subset of items focused on individual health and functioning |
| National Comprehensive Cancer Network – Distress Thermometer (NCCN-DT) | The NCCN-DT consists of a single item with instructions to rate distress over the past 7 days on a scale of 0–10, with higher scores indicating higher distress |
| Beck Depression Inventory (BDI) | The BDI–Short Form is a widely used depression scale that consists of 13 items that measure characteristic attitudes and symptoms of depression |
| Brief Edinburgh Depression Scale | 6-item inventory rated on a four-point Likert-type scale designed to measure depression in those in the advanced stages of cancer |
| Brief Symptom Inventory-18 (BSI-18) | BSI-18 is a self-report scale widely used to assess psychological symptoms in cancer survivors |
| Profile of Moods State–Short Form (POMS-SF) | 16-item survey that assesses mood states |
| Psychosocial Screen for Cancer (PSSCAN) | 21-item tool used to identify the psychosocial needs of patients with cancer |
| Hospital Anxiety and Depression Scale (HADS) | 14-item questionnaire that assesses anxiety and depressive symptoms in medical settings |
A 2017 study that looked at 55 cancer programs in the United States and Canada found that 84% of cancer programs used the NCCN Distress Thermometer and Symptom Checklist to screen their patients for psychosocial distress. NCCN distress-management guidelines are useful in outlining recommendations for supporting patients with mild distress and providing a pathway for referral to supportive psychosocial resources. Referral to an oncology social worker, financial navigator, or psychologist or psychiatrist, preferably one who has experience working with cancer survivors, can be very beneficial for patients who are experiencing depression and anxiety. Counseling and cognitive-behavioral therapy can be beneficial for cancer survivors who are dealing with distress. Pharmacologic treatment may be indicated, but if prescribing medication, it is recommended that referral and collaboration with a prescribing mental health professional be considered.
Fatigue
Fatigue is a common complaint among cancer survivors. Wang et al. found that about one-third of cancer survivors with breast, prostate, colorectal, or lung cancer diagnoses reported moderate to severe levels of fatigue after treatment. Cancer-related fatigue can be difficult to quantify and is usually multifactorial, impacted by surgery, chemotherapy, and radiation. It can also be caused by chronic pain, cardiovascular or endocrine comorbidities, anemia, psychosocial distress, sleep disturbances, cognitive dysfunction, and side effects from medications. When breast cancer survivors complain of fatigue post-treatment, the presence of depression and anxiety should be assessed as they are the most common psychiatric comorbidities that occur in individuals with cancer-related fatigue, even after treatment.
There are a number of screening tools that can be used to assess cancer-related fatigue, including the Fatigue Symptom Inventory (FSI), the Multidimensional Fatigue Inventory (MFI), and the Multidimensional Fatigue Symptom Inventory (MFSI). The ASCO guidelines recommend that all patients be screened for fatigue as clinically indicated, and at least on a yearly basis. As part of that assessment, sleep patterns should be evaluated. Carpenter et al. found that 73% of breast cancer survivors experienced poor sleep quality and high sleep disturbance. There are a number of medications that can be used to treat insomnia, but they all have potential side effects, including the risk of dependence, and ideally should only be used in the short term. Meditation, yoga, acupuncture, and cognitive-behavioral stress management can also yield positive results. Cognitive-behavioral therapy sessions with a mental health therapist have been found to be beneficial and are also now available via mobile apps. Use of psychostimulants and other wakefulness agents such as modafinil should not be used in breast cancer survivors except under special circumstances. These medications can be effectively used to manage fatigue in patients with advanced disease or those receiving active treatment. However, there is limited evidence of their effectiveness in reducing fatigue in patients after active treatment who are currently disease free. The American Academy of Sleep Medicine has developed guidelines for the treatment of insomnia in adults Table 13.5 ). Nonpharmacologic interventions to help patients sleep should be recommended, including:
- •
Go to bed at the same time each night and get up at the same time each morning, including on the weekends.
- •
Keep the bedroom quiet, dark, relaxing, and at a comfortable temperature.
- •
Do not use any electronic devices, such as TVs, computers, and smart phones, in the bedroom.
- •
Avoid large meals, caffeine, and alcohol before bedtime.
- •
Get some exercise during the daytime.
| Medication | Sleep Latency | Quality of Sleep | Side Effects | Sleep Onset vs. Sleep Latency |
|---|---|---|---|---|
| Eszopiclone |
| Moderate to large improvement | Dizziness, dry mouth, headache, somnolence, and unpleasant taste | Onset and latency |
| Ramelteon | 9 min compared to placebo for sleep onset | No improvement | Headache, nausea, upper respiratory infection, and nasopharyngitis | Onset |
| Temazepam | 37 min compared to placebo for sleep onset 99 min of sleep improvement | Small improvement | Headache, blurred vision, depression, and confusion | Onset and latency |
| Triazolam | 8 min compared to placebo for sleep onset | Moderate improvement | Somnolence | Onset |
| Zaleplon | 10 min compared to placebo for sleep onset | No improvement | Headache, asthenia, neurasthenia, pain, fatigue, and somnolence | Onset |
| Zolpidem |
| Moderate improvement | Amnesia, dizziness, sedation, headache, nausea, and taste perversion (altered or unpleasant taste) | Onset and latency |
| Doxepin | 26–32 min of sleep improvement | Small to moderate | Headache, diarrhea, somnolence | Latency |
| Suvorexant | 10 min of sleep improvement | Not reported | Somnolence | Latency |
| Trazodone |
| No improvement | Headache, somnolence | Onset and latency |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree