Chapter 16 Autoimmune Hemolytic Anemia
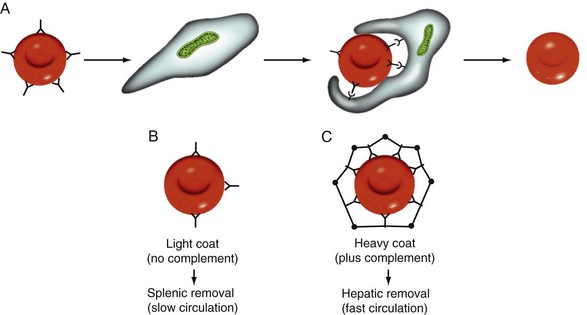
Figure 16-1 MECHANISM OF EXTRAVASCULAR HEMOLYSIS IN AUTOIMMUNE HEMOLYTIC ANEMIA.
(From Cunnigham MJ, Silberstein LE: Autoimmune Hemolytic Anemia. In Hoffman R, Benz EJ Jr, Shattil SJ, et al, eds: Hematology: Basic principles and practice, ed 4, 2005, Philadelphia, Elsevier.)
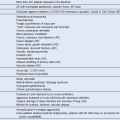
Table 16-1 Properties and Specificities of Red Blood Cell Autoantibodies
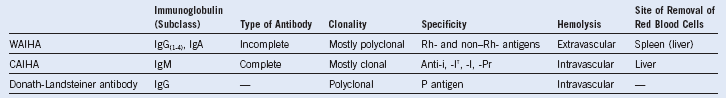
CAIHA, Cold autoimmune hemolytic anemia; Ig, immunoglobulin; WAIHA, warm autoimmune hemolytic anemia.
Four Important Questions for the Diagnosis and Management of Autoimmune Hemolytic Anemia
Question 1: Hemolytic anemia? The basic features of hemolytic anemia are reticulocytosis, low haptoglobin levels, elevated indirect bilirubin, and elevated LDH.
Question 2: Autoimmune hemolytic anemia? A direct DAT is initially performed with a polyspecific antibody to detect IgG or complement C3d bound to RBCs. If the DAT result is positive, the diagnosis of AIHA is established.
Question 3: Warm or Cold Autoimmune Hemolytic Anemia?
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree