Part A: Curriculum Plan |
Program Purpose |
Develop knowledge and clinical skills in PICC nursing care and prevention of CLABSI. |
Learning Objectives |
At the end of the session, the participant will be able to:
Describe a PICC.
Identify one action to prevent CLABSI in PICCs.
Perform a dressing change for a PICC.
Administer medication through a PICC.
|
Instructional Methods |
Audience response participation system
Presentation
Discussion
Video
Simulation (task trainer) |
Target Audience |
Infusion Nurses |
Instructional Tools for PICC Education Learning Stations |
Dressing change learning station:
PICC arm with catheter
Alcohol swabs
Waterless hand sanitizer
Gloves
Transparent semipermeable chlorhexidine gluconate dressing kit |
Medication administration learning station:
PICC arm with catheter
Alcohol swabs
Waterless hand sanitizer
Gloves
IV tubing primary and secondary
10 mL 0.9 NS prefilled syringes
Heparin prefilled syringe (based upon policy for PICC locking)
|
Instructor Resources for Planning Curriculum Content |
Alexander, M., Corrigan, A.M., Gorski, L.A., Hankins, J., & Perucca, R. (2010). Infusion nursing: An evidence-based approach (3rd ed.). St Louis, MO: Saunders Elsevier.
Alexander, M., Corrigan, A.M., Gorski, L.A., & Phillips, L. (2014). Core curriculum for infusion nursing (4th ed.). Philadelphia, PA: Lippincott Williams & Wilkins.
Bartock, L. (2010). An evidence-based systematic review of literature for the reduction of PICC line occlusions. Journal of the Association for Vascular Access, 15, 58-63.
Bucher, L., & Sanderson, L.V. (2011). Peripherally inserted central catheter. In D. Wiegand (Ed.), AACN procedure manual for critical care (6th ed., pp. 763-774). Philadelphia, PA: Saunders.
Camp-Sorrell, D. (2011). Access device guidelines: Recommendations for nursing practice and education (3rd ed.). Pittsburgh, PA: Oncology Nursing Society.
CDC. (2011). Guidelines for the prevention of intravascular catheter-related infections. http://www.cdc.gov/hicpac/pdf/guidelines/bsi-guidelines-2011.pdf
Infusion Nurses Society. (2011). Infusion nursing standards of practice. Journal of Infusion Nursing, 34(15), S1-S110.
Organizational policy
|
Preclass Learner Assignment |
Instructor could assign an article for participants to review. |
Kirkpatrick’s Evaluation |
Level 1: Class evaluation
Level 2: Preevaluation of knowledge compared to postevaluation of knowledge using audience response system |
Part B: Content |
Time |
Objectives |
Content |
Instructional Methods |
15 minutes |
Introduction |
Introduction of instructor
Ice breaker: name and first paying job
Review locations of restrooms and personal electronic device expectations
Review objectives
Complete preevaluation questions using audience response participation system
|
Audience response participation system |
15 minutes |
Describe a PICC |
PICC suggested content:
Definition
Arm anatomy for insertion sites: cephalic, basilic, median cubital, and brachial veins
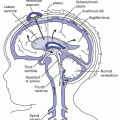
Heart anatomy: chambers, superior/inferior vena cava, circulation, tip rests in the distal superior vena cava
Rationale for use
Insertion sites, contradictions for placement, and what to avoid when a patient has a PICC
Catheter: single or multilumen, power injectable, staggered lumen exits, various gauges and lengths, 10-mL syringe or greater for medication/blood draw/flushing
|
Arm diagram
Heart diagram
Single- and multilumen PICC and power injectable PICC |
15 minutes |
Identify one action to prevent catheter-associated bloodstream infections in PICCs |
Activity from audience response participation system suggested content:
Q: Audience response: What one patient demographic increases risk for infection?
A: Age: premature infants and patients older than 65
Q: Audience response: Name this potential PICC complication.
A: Phlebitis, infiltration, extravasation, infection, air embolism, catheter embolism, venous thrombosis, and malposition. Include content on why the complication occurs and prevention strategies CLABSI prevention and standard assessment-suggested content:
CLABSI prevention guidelines from the CDC include health care provider training, correct hand hygiene, use of maximal barrier protection, use of chlorhexidine gluconate solution for skin antisepsis, and daily review of continuation of need for access device.
Standardized assessment: visual condition of site, palpation of site, patient discomfort at insertion site or arm, external catheter length, integrity of device, closed secure system, signs/symptoms of infection
|
Audience response system slides
Pictures of complications
Demonstrate with task trainer |
30 min |
Perform a dressing change for a PICC |
Dressing suggested content: aseptic application, product integrity, transparent semipermeable dressing, occlusive, site label, device secure, and frequency of dressing change
Use a standardized checklist
Learners to perform PICC dressing change with removal of dressing, placement of new dressing, and documentation based upon agency policy
|
Video demonstration and show materials
Simulation: task trainer and materials |
30 min |
Administer medication through a PICC |
Medication administration suggested content: product integrity, add-on devices only when needed, access port integrity, aseptic technique, venous blood return and patency, flushing PICC pre- and postmedication administration, use of heparin or antireflux device based upon agency policy
Use a standardized checklist
Learners to perform PICC medication administration with flushing/locking of PICC line based upon agency policy
|
Video Demonstration and show materials
Simulation: task trainer and materials |
10 min |
End of class |
Review objectives
Complete postevaluation using audience response participation system |
Audience response participation system |
 EVIDENCE FOR PRACTICE
EVIDENCE FOR PRACTICE PATIENT SAFETY
PATIENT SAFETY RESEARCH ISSUE
RESEARCH ISSUE