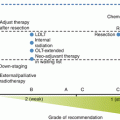
Concept
Resection + intra-arterial chemotherapy vs. resection alone
N
51
Access
Catheter via A. femoralis in truncus coeliacus
Therapy
d1: 10 mg/m2 mitoxantrone (over 1 h)
d2–4: 170 mg/m2 FA (over 10 min) + 600 mg/m2 5-FU (over 2 h)
d5: 60 mg/m2 cisDDP (over 1 h)
Frequency
Every 4 weeks
Survival
23 mo vs. 11 mo
R0-resection (at 4 years): 54 vs. 10 %
Hepatic metastasis
Reduction to 17 %
Toxicity
No severe local side effects
Conclusion
The results demonstrate that CAI is well tolerated, reduces the risk of liver metastasis, and increases the survival time of pancreatic cancer patients
Cantore et al. (2006) [2]
Concept | Resection + intra-arterial chemotherapy ±IV gemcitabine |
N | 47 |
Access | Catheter via A. femoralis in truncus coeliacus |
Therapy | 5FU 750 mg/m2, leucovorin 75 mg/m2, epirubicin 45 mg/m2, carboplatin 225 mg/m2 (FLEC regimen) |
Frequency | Every 3 weeks |
Survival | Median disease-free-survival: 16.9 months, median overall survival: 29.7 months |
Hepatic metastasis | 62 % of recurrence |
Toxicity | Main grade 3 toxicity related to HAI was only nausea/vomiting in 4 % of the patients |
Conclusion | FLEC regimen with or without gemcitabine is active with a very mild toxicity and results are very encouraging in an adjuvant setting |
Hayashibe et al. (2007) [3]
Concept | Resection + intra-arterial chemotherapy vs. resection alone (non randomized) |
N | 22 |
Access | Catheter via A. femoralis in proper hepatic artery |
Therapy | 5FU 500 mg/m2 180 min infusion + cisplatin 10 mg/m2 |
Frequency | weekly “as much as possible” |
Survival | 15.8 mo vs. 13.4 mo NS |
Hepatic metastasis | 33 % in the treated group vs. 54 % in the control group |
Toxicity | No severe local side effects |
Conclusion | In patients with pancreatic cancer who underwent the curative operation, the intra-arterial adjuvant chemotherapy had the tendency to suppress the rate of liver metastasis and improve cumulative survival |
7.2.2 Metastatic Disease
Homma and Niitsu (2002) [4]
Concept | Hepatic arterial infusion |
N | 31 |
Access | Catheter into A. femoralis to celiac artery |
Therapy | 20 mg/m2 cisDDP (d1, 3, 5) + 500 mg/m2 5-FU (d1–7) |
Frequency | Every 4 weeks |
Survival | 1, 2, 3 y: 67, 31, 14 % |
Median survival: 16 mo | |
Toxicity | Cytopenia (grade II): N = 11, transient nausea, mild anorexia |
Conclusion | In patients with stage IV advanced pancreatic carcinoma, arterial infusion chemotherapy after hemodynamic change was found to be effective against both primary tumors and metastatic liver lesions |
Vogl et al. (2006) [5]
Concept | Intra-arterial dose finding of gemcitabine +/6 starch microspheres |
N | 24 |
Access | Catheter into A. femoralis placed in the truncus coeliacus |
Therapy | HAI: initial dose, 1,000 mg/m2 (d1 + d8) every 2 weeks (max. 6 cycles); dose steps, 200 mg/m2 (till MTD) |
TACE: initial dose, HAI-MTD – 1 dose-step, + microspheres | |
MTD | HAI: 1,600 mg/m2 |
TACE: 1,800 mg/m2 | |
Response rates | TtP |
HAI: 4 mo | |
TACE: 7 mo | |
Survival | Median survival |
HAI: 14 mo | |
TACE: 20 mo | |
Toxicity | Myelosuppression (grade III) |
Conclusion | This clinical study indicates that the intra-arterial application of gemcitabine with doses higher than the recommended 1,000 mg/m2 is well tolerated if combined with microspheres and yields respectable results in patients who do not respond to systemic chemotherapy |
Cantore et al. (2003) [6]
Concept | Intra-arterial chemotherapy vs. IV gemcitabine |
N | 71 vs. 67 |
Access | Catheter via A. femoralis in truncus coeliacus |
Therapy | 5FU 1,000 mg/m2, leucovorin 100 mg/m2, epirubicin 60 mg/m2, carboplatin 300 mg/m2 (FLEC regimen) |
Frequency | Every 3 weeks |
Response rate | 14 % for FLEC vs. 5.9 % for gemcitabine (NS) |
Survival | Median overall survival: 7.9 months in the FLEC group vs. 5.8 months in the gemcitabine group (p = 0.13) |
Toxicity | Main grade 3 toxicity related to IAC was only nausea/vomiting in 4 %; regarding gemcitabine, grade 3 toxicities were anemia 8 %, leukopenia 8 %, thrombocytopenia 17 %, and nausea/vomiting 4 % |
Conclusion | FLEC regimen with or without gemcitabine is active with a very mild toxicity and results are very encouraging in an adjuvant setting |
Ikeda et al. (2007) [7]
Concept | HAI + IV therapy |
N | 33 |
Access | Port system (catheter into A. subclavia or right A. femoralis) |
Therapy | IV: 1,000 mg/m2 gemcitabine (over 30 min) d1, 8, 15 |
HAI: 250 mg/m2 5-FU d1–5 | |
Frequency | Every 4 weeks |
Response rates | PR: N = 8 (24 %), PD: 9 (27 %) |
Survival??? | |
Toxicity | Leukopenia (grade III), N = 8; thrombocytopenia, N = 6; non-hematologic (grade III), N = 5 |
Conclusion | For patients with advanced pancreatic cancer, HAI with systemic chemotherapy appeared to be effective and may prolong survival |
Azizi et al. (2011) [8]
Concept | TACE for liver metastases |
N | 32 |
Access | Femoral arterial access, advanced into the relevant segmental artery |
Therapy | 8 mg/m2 MMC + 40 mg/m2 cisDDP + 1,000 mg/m2 gemcitabine + lipiodol + 200–450 mg DSM |
Frequency | Every 4–8 weeks |
Response rates | PR: N = 3 (9 %), SD: N = 23 (72 %), PD: N = 6 (19 %) |
Survival | Median survival: 16 mo (SD: 20 mo, PD: 5 mo) |
Toxicity | No major complications |
Conclusion | Repetitive TACE resulted in a relevant response for the control of liver metastases of pancreatic cancer with respectable median survival time |
Recommendations
Locoregional treatment of liver metastases of pancreatic adenocarcinoma remains a matter of research. It is conceptually interesting for the treatment of pancreatic carcinoma even if recent polychemotherapy has given interesting results (FOLFIRINOX, gemcitabine + nab-paclitaxel). In adjuvant setting the data are scarce, but considering the high level of liver recurrence after surgical excision of pancreatic cancer and even if systemic treatment has given some hope, it could be considered in future trials.
7.3 Liver Metastases of Melanoma
7.3.1 Hepatic Arterial Infusion
Becker et al. (2002) [9]
Concept | HAI or IV of fotemustine + SC IL-2 + IFN |
N | 48 |
Inclusion criteria | Liver and extrahepatic metastases |
Therapy | d1: IA 100 mg/m2 fotemustine (over 60 min) or |
IV 100 mg/m2 fotemustine (over 15 min) | |
d31–33: SC 10 × 106 IU/m2 IL-2 (2×/d) | |
d36, 38, 40: SC 10 × 106 IU/m2 IFN + SC 5 ×106 IU/m2 IL-2 | |
Response rates | RR: 15 % (N = 7); (5 from the HAI group) |
HAI vs. IV: 22 vs. 8 % | |
CR: N = 1; PR: N = 6 | |
Survival | 8.5 mo (HAI vs. IV: 369 vs. 349 d) |
Toxicity | Thrombocytopenia, leukopenia (more prominent systemic side effects in the IV group) |
Conclusions | Although objective responses were more frequent within the cohort receiving intra-arterial fotemustine, this difference did not translate into a significant benefit in overall survival. Of note, this overall survival is much longer than that repeatedly reported for stage IV uveal melanoma not treated with fotemustine, suggesting a therapeutic activity of this cytostatic drug even after systemic administration |
Peters et al. (2006) [10]
Concept | HAI (retrospective study) |
N | 101 |
Inclusion criteria | Chemotherapeutic naive patients |
Therapy | 100 mg/m2 fotemustine (over 4 h) |
Every 4 weeks | |
Response rates | RR: 36 % |
CR: N = 15; PR: N = 21; SD: N = 48 | |
TtP: 9 mo | |
Survival | Median survival: 15 mo |
1 y, 2 y, 3 y: 67, 29, 12 % | |
Toxicity | Grade III and IV: 11 % (mainly hematoxicity), grade II: (mainly hematoxicity) |
Complications with catheters: N = 21 (thrombosis, dislocation, obstruction, leakage) | |
Conclusions | Locoregional treatment with fotemustine is well tolerated and seems to improve outcome of this poor prognosis patient population |
Siegel et al. (2007) [11]
Concept | HAI (retrospective study) |
N | 30 (18 uveal) |
Inclusion criteria | Liver-limited disease |
Therapy | 100 mg/m2 fotemustine (over 4 h) |
Every 4 weeks | |
Response rates | RR: 30 % |
PR: N = 9; SD: N = 10 | |
TtP: 9 mo | |
Survival | Median survival: 14 mo |
1 y, 2 y, 3 y: 67, 29, 12 % | |
Toxicity | ≥ Grade III thrombocytopenia/30 %; ≥ grade 3 neutropenia: 7 % |
Conclusions | Hepatic arterial fotemustine chemotherapy was well tolerated. Meaningful response and survival rates were achieved in ocular as well as cutaneous melanoma |
Voelter et al. (2008) [12]
Concept | HAI (prospective study, historical control) |
N | 22 |
Inclusion criteria | High risk of liver metastases patients |
Therapy | 100 mg/m2 fotemustine (over 4 h) |
Every 3 weeks | |
Response | NA – adjuvant treatment |
Survival | Median survival: 9 years vs. 7.4 years for control group |
5-year survival: 75 % vs. 56 % | |
Toxicity | 50 % grade 3–4 hepatotoxicity including one patient with cholangitis 8 years later |
Conclusions | Although these data suggest a survival benefit, it was not statistically significant. Confirming such a benefit would require a large, internationally coordinated, prospective randomized trial
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|