| Host defense factor | Example disease state |
|---|---|
| Barrier | |
| Gastric acid | Achlorhydria (PPI, HIV, gastric surgery) |
| Mucosal integrity | Mucositis (chemotherapy) |
| Intestinal motility | |
| Peristalsis | Blind loop, antimotility drugs, hypomotility states (diabetes, scleroderma) |
| Commensal microflora | Antibiotics, age extremes |
| Sanitation | Contaminated water |
| Intestinal immunity | |
| Phagocytic | Neutropenia |
| Cellular | HIV |
| Humoral | IgA deficiency |
Abbreviations: PPI = proton pump inhibitor; HIV = human immunodeficiency virus; IgA = immunoglobulin A.
Virulence factors play a complementary role in acute infectious diarrhea. Whether an individual ingests an inoculum sufficient to establish clinical gastroenteritis is directly related to the organisms, community sanitation, and personal hygiene. Most organisms require an inoculum of 105 to 108 to establish infection. Exceptions include Shigella and protozoa such as Giardia, Cryptosporidium, and Entamoeba, which may cause diarrhea when only 10 to 100 organisms are ingested. Certain bacteria may produce toxins, which lead to a variety of clinical syndromes, and include enterotoxin (watery diarrhea), cytotoxin (dysentery), and neurotoxin. Botulinum toxin is the classic example of a preformed neurotoxin, but interestingly, both Staphylococcus aureus and Bacillus cereus also produce neurotoxins, which act on the central nervous system to produce emesis. Adherence and invasion factors facilitate colonization and contribute to virulence. Various forms of Escherichia coli express the gamut of virulence factors (Table 49.2).
| Virulence factors | Examples |
|---|---|
| Inoculum size | Shigella, Entamoeba, Giardia |
| Adherence | Cholera, EPEC |
| Invasion | Shigella, Salmonella typhi, Yersinia, EIEC |
| Toxins | |
| Enterotoxin | Cholera, Salmonella, ETEC |
| Cytotoxin | Shigella, Clostridium difficile, EHEC |
| Neurotoxin | Clostridium botulinum, Staphylococcus aureus, Bacillus cereus |
Abbreviations: EPEC = enteropathogenic Escherichia coli; EIEC = enteroinvasive E. coli; ETEC = enterotoxigenic E. coli; EHEC = enterohemorrhagic E. coli.
Clinical syndromes
The acute infectious diarrheas can be divided into noninflammatory, inflammatory, and invasive (Table 49.3). Overall in the United States, the most common bacterial or protozoal pathogens in the acute setting are Campylobacter, Salmonella, Shigella, E. coli O157:H7, and more recently, Clostridium difficile. While the majority of noninflammatory episodes are viral, the more severe cases are often bacterial. The bacteria causing a noninflammatory diarrhea, such as Vibrio cholerae and enterotoxigenic E. coli (ETEC), typically secrete an enterotoxin, which affects the small intestine, producing a large volume of watery diarrhea without fecal leukocytes. Most forms of viral gastroenteritis fall into this group. The four most common enteric viral infections are norovirus, rotavirus, adenovirus, and astrovirus. The three most common parasites responsible for noninflammatory diarrhea are Cryptosporidium, Giardia, and Cyclospora.
| Noninflammatory | Inflammatory | Invasive | |
|---|---|---|---|
| Syndrome | Watery diarrhea, emesis | Dysentery | Enteric fever |
| Site | Small intestine | Colon | Ileum, colon |
| Stool | |||
| Volume | Large | Small | Small |
| Fecal WBCs | Absent | Present | Present |
| Common organisms | |||
| Bacteria | Vibrio cholerae | Shigella spp. | Salmonella typhi |
| ETEC | Salmonella spp. | Yersinia spp. | |
| Campylobacter jejuni | Brucella | ||
| Viruses | Rotavirus | — | — |
| Norovirusa | |||
| Adenovirus | |||
| Astrovirus | |||
| Parasites | Giardia | Entamoeba | Entamoeba |
| Cryptosporidium | |||
Abbreviations: WBC = white blood cell; ETEC = enterotoxigenic E. coli; EIEC, enteroinvasive E. coli.
a Formerly known as the Norwalk agent or calicivirus.
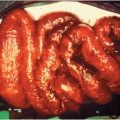
The inflammatory diarrheas typically affect the colon, causing frequent small-volume stools, often with fecal white cells and either occult or gross blood. Fever, tenesmus, and bloody diarrhea are characteristic of dysentery. A pathogen is identified in about one-fifth of cases of bloody diarrhea, most commonly, enterohemorrhagic (EHEC) E. coli O157:H7, Shigella, Campylobacter, and Salmonella. Certain bacteria that cause inflammatory diarrhea produce cytotoxins. The invasive diarrheas may be considered a subset of the inflammatory diarrheas with invasion of the intestinal mucosa, and a propensity to cause bacteremia and distant disease. Salmonella typhi is the prototype. Typhoid bacteria are taken up and proliferate within the Peyer’s patches of the distal ileum, then disseminate and multiply in the reticuloendothelial system to produce systemic disease. E. coli O157:H7 in human and animal studies has been shown to affect both the small and large intestines often with hemorrhage noted throughout. Both the Shigella and the EHEC pathogens have been associated with sequelae such as hemolytic-uremic syndrome (HUS) and thrombotic thrombocytopenic purpura (TTP).
Patients with neutropenia, particularly with an absolute neutrophil count <500/mm3 and secondary to immunodeficiency or cytotoxic medications (e.g., bone marrow transplantation) can develop neutropenic enterocolitis or typhlitis (from typhlon, the Greek term for cecum). In these patients, cytotoxic mucosal injury and neutropenia affect host defenses and mucosal integrity to allow invasion and produce fever, abdominal pain (often right lower quadrant), watery or bloody diarrhea, and thickening of the bowel wall on computed tomography (CT) imaging.
Certain populations of patients with gastroenteritis merit surveillance because of the organisms involved, the potential for severe disease, and the possible need for intervention (Table 49.4). Foodborne disease should be considered in outbreaks of acute GI symptoms affecting two or more persons. The most common causes include Salmonella species, Campylobacter, Shigella species, EHEC (Shiga toxin), B. cereus, and the parasites Cryptosporidium and Cyclospora (see Chapter 50, Food poisoning). The microbial pathogens responsible for travelers’ diarrhea are dependent upon the region visited, with some of the most common being enteroaggregative E. coli (EAEC), ETEC, Salmonella, Campylobacter, and Shigella (see Chapter 121, Travelers’ diarrhea). Patients with advanced acquired immunodeficiency syndrome (AIDS), particularly with CD4 counts <50/µL, are predisposed to a number of unique infections (microsporidia, Cyclospora, Cystoisospora – formerly known as isosporiasis, cytomegalovirus) which may be chronic, and more severe manifestations of otherwise common infections (Salmonella, Campylobacter, Cryptosporidium). Acute infectious proctitis, which is often sexually transmitted, leads to tenesmus, hematochezia, and rectal pain. Syphilis, gonorrhea, and chlamydia are additional organisms to consider. The incidence of sexually transmitted proctitis is decreasing in the AIDS era with safer sex practices. Other important subpopulations include patients with antibiotic-associated diarrhea, especially those from hospitals or chronic care facilities (see Chapter 51, Antibiotic-associated diarrhea). Helicobacter pylori is the most common chronic bacterial infection in the world, and is associated with chronic gastritis, peptic ulcer, gastric adenocarcinoma, and gastric MALToma (Chapter 138, Helicobacter pylori infection).
| Population | Bacteria | Viruses | Parasites | Other |
|---|---|---|---|---|
| Food poisoning | Salmonella Staphylococcus aureus Shigella Clostridium perfringens Bacillus cereus Listeria | Norwalk Hepatitis A | Trichinella Giardia Cryptosporidium | Ciguatera Histamine fish |
| AIDS | Salmonella Campylobacter Shigella MAC | CMV | Cryptosporidium Cystoisospora belli Microsporidia | AIDS Enteropathy |
| Travelers’ diarrhea | Escherichia coli ETEC Shigella Aeromonas E. coli, other | Rotavirus | Giardia Cyclospora | No pathogen (40%) |
| Acute proctitis | Neisseria gonorrheae Chlamydia Treponema pallidum Shigella Salmonella | HSV Condyloma, HPV CMV | Entamoeba Cryptosporidium |