22.1 Introduction
Falls and fractures in older people are a major and increasing public health issue, affecting 150 000– 200 000 people each year in the UK and about 3 million people worldwide. A bone’s tendency to fracture depends on the strength of the bone and the amount of trauma applied to it. In the majority of cases in the elderly, these fractures are attributable at least in part to structural weakness of the skeleton referred to as osteoporosis. The roots of this problem lie many years before it becomes manifest as a fracture, and involve growth and nutrition across the whole lifespan, starting in utero. This chapter describes the epidemiology of osteoporosis, the personal and social impact of the disease process, the biology of bone growth and repair, and the major nutritional elements involved in the maintenance of bone health.
22.2 Definition
The term osteoporosis (literally porous bone) describes a systemic skeletal disorder characterized by low bone mass and microarchitectural deterioration of bone tissue, leading to increased propensity to fractures (Figure 22.1). Recognition of increased fragility of the bones in older women dates back to surgical accounts in the nineteenth century literature, but it is only since the mid-twentieth century that osteoporosis has been described as a specific entity and its importance as a cause of fracture appreciated. Much of the impetus for our developing understanding of the condition has been linked to the development of radiological techniques that allow identification of osteoporosis without the highly invasive procedure of bone biopsy. Once a workable clinical definition of osteoporosis based on radiological techniques had been established by the World Health Organization (WHO) it became practicable to conduct clinical studies including pharmaceutical trials of treatments for osteoporosis (Figure 22.2). It is important to realize, however, that although the WHO definition is based on bone density measurement, bone density is just one risk factor for susceptibility to fracture.
Figure 22.1 Bone strength and trauma. RTA: road traffic accident.
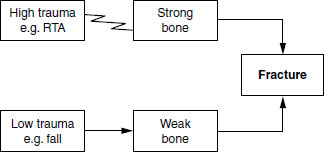
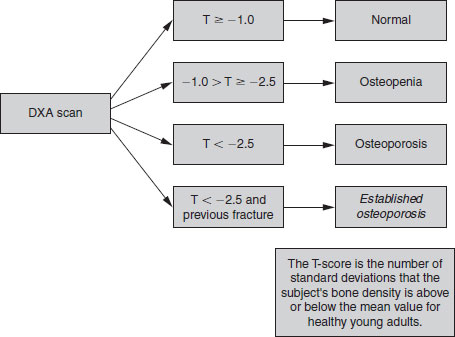
Figure 22.2 WHO (1994) definition of osteoporosis by T-score. DXA: dual-energy X-ray absorptiometry.
22.3 Epidemiology: the scale of the problem
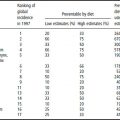
It is clear from large population studies in North America and Europe that osteoporosis-related fracture is common in both genders throughout the developed world. Analysis of hospital discharge records shows that there are now more than 150 000 osteoporosis-related fractures in the UK each year, of which over 60 000 are hip fractures. In the USA, more than 1.2 million osteoporosis-related fractures are reported annually. A reasonable estimate of the current annual incidence of hip fractures worldwide would be 6 million, extrapolating from known rates in populations of various ethnic and social compositions. The incidence of osteoporotic fracture has been increasing since the condition was first recorded, and although the most influential factor has been change in the age distribution of the populations studied, there has been a separate and rather worrying increase in age-specific rates as well. Various explanations have been put forward; the most credible is the decrease in daily weight-bearing physical exertion resulting from the general movement away from agriculture and heavy industry. The incidence of osteoporosis has not been widely studied among agrarian societies (whose people often have more pressing health concerns). Future projections show a worrying increase: the predicted annual incidence of hip fractures in Europe and North America will be over 1.3 million by the year 2025.
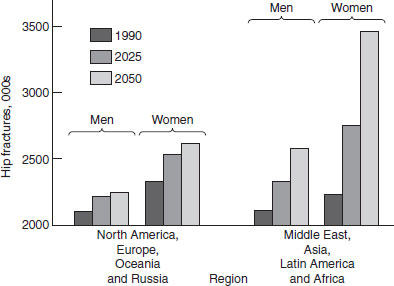
So far, osteoporosis has been very much a disease of Western and Westernized societies of white European origin, but this is certain to change as a result of increased longevity, cultural change and growth of other risk factors among black and Asian people. Such populations have not been studied as diligently, and fracture risk estimates are often based on fairly small and perhaps unrepresentative samples. Nonetheless, it is reasonable to accept that non-European races are relatively protected against osteoporosis, partly because of a higher average bone density in people of black African descent, but mostly because of a lower fracture rate at any given bone density in both Africans and Asians. The explanation for this latter finding is unclear, but if it relates to cultural rather than racial factors (physical exertion, low rates of smoking, etc.) then one would expect the same increase in age-specific rates already seen in white Westerners to show up in due course. Population expansion is a factor in this as in all other public health issues, but changes in age distribution may have a greater effect on the impact of osteoporosis on a society. As life expectancy increases and birth rates fall – the pattern associated with accession to “developed” status – the majority of fractures in 2025 will be in the developing world (Figure 22.3).
Figure 22.3 Predicted increase in osteoporosis worldwide over the next 50 years. Reproduced with permission for Cooper et al. (1992). © Springer Publishing Company, Inc.
Etiology
A low bone mass may result from a failure to achieve normal bone accrual during development, or from excessive loss. Peak bone mass is reached in the early twenties, and there is evidence that factors such as lack of exercise, poor intake of vitamin D and calcium, delayed puberty, smoking and excess alcohol consumption adversely affect bone mineral accrual. Importantly, recent work has shown that maternal factors can influence bone growth in utero, and it is becoming apparent that influences in early life are also an important determinant of later fracture risk (see Intrauterine programming in Section 22.4). In women estrogen protects against bone loss, so the rate of bone resorption increases after the menopause, leading to postmenopausal osteoporosis. A late menarche increases the risk of fracture in later life. Genetic factors play a role, but only account for up to 60% of variance in bone mineral density (BMD). There is no one gene that account for this: several genes, such as the vitamin D receptor, collagen 1A1 and insulin-like, growth factor-1 (IGF-1), play a part, but studies have demonstrated only a small effect. Recent work suggests an interaction between polymorphisms in the vitamin D receptor gene and the early life environment, influencing bone mass in later life. Drug treatment with corticosteroids is an important cause of secondary osteoporosis. Systemic diseases that lead to low bone mass are listed in Table 22.1.
Presentation
Osteoporosis is asymptomatic until fractures occur. There are three ways in which the possible diagnosis of osteoporosis may be raised: incident low-trauma fracture, radiological evidence of osteopenia and presentation with risk factors. Diagnosing osteoporosis on the basis of a fracture is rather like diagnosing hypertension on the basis of a stroke; much of the damage has been done and intervention can only ameliorate the effects of established disease. In a perfect world, osteoporosis would be detected at a presymptomatic stage and fractures prevented, but until recently the diagnosis was often not considered even after a fracture. People with osteoporosis are at risk of fractures at any site exposed to trauma, and will suffer a fracture at a lower level of transmitted energy than people who do not have osteoporosis.
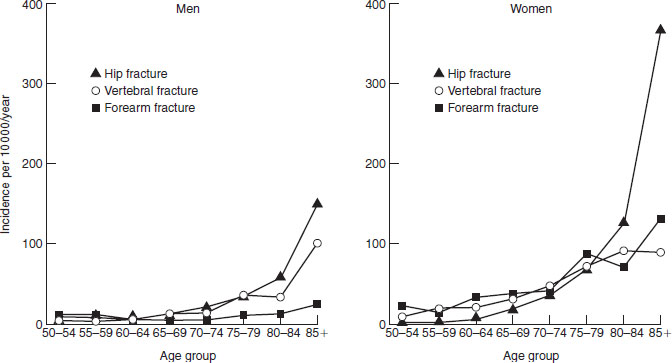
The most widely recognized osteoporotic fractures are those of the hip, wrist and vertebral body, but in adults osteoporosis is a principal or contributory factor in the majority of fractures at all sites other than the facial bones and skull. The relative contribution of trauma and bone fragility in any given fracture is often difficult to estimate, although in circumstances such as road traffic accidents or falls out of bed one can be fairly clear where the problem lies. The classic sites for osteoporosis-related fracture have a higher than average percentage of trabecular bone, and fractures at such sites are associated with conditions causing rapid bone turnover, the most important of which is the menopause. The slowly progressive involutional osteoporosis of late life has no particular association with specific fractures, but it has been estimated that osteoporosis is associated with over 90% of hip fractures in the elderly (Figure 22.4).
Table 22.1 Risk factors for osteoporosis in late life
| Untreatable | Treatable | Associated diseases |
| Age | Hysterectomy/oophorectomy | Hyperthyroidism |
| Female gender | Low peak bone mass | Hyperparathyroidism |
| Family history | Low calcium/vitamin D intake | Myeloma |
| Previous fracture | Prolonged immobilization | Inflammatory arthritis |
| Early menopause | Gonadal failure (men) | Malabsorption |
| Low peak bone mass | Corticosteroid use | Celiac disease |
| Smoking | Inflammatory bowel disease | |
| Excess alcohol | Chronic renal failure | |
| Anorexia nervosa |
Figure 22.4 Incidence by age of osteoporotic fracture at the hip, wrist and spine in the UK. Reprinted from Cooper and Melton (1992) with permission from Elsevier.
Vertebral fracture
Vertebral fractures are often silent, but may present with acute onset of severe back pain in the midthoracic or upper lumbar region, associated with heavy lifting or a fall. There are many other causes of back pain and the diagnosis is often missed, particularly in men. However, in postmenopausal women it is very likely that such symptoms are due to osteoporotic fracture. Pain is typically severe for 6–8 weeks, subsiding to a dull ache and remitting completely after a few months. Subsequent fractures are associated with progression to chronic pain, height loss and kyphosis. In some cases, however, symptoms may be minimal until several vertebrae have collapsed, leading to the characteristic “dowager’s hump”. Height loss may exceed 20 cm in severe cases, compromising respiratory function and leading to repeated chest infections. Early mortality from vertebral fractures is negligible, but sufferers have a persistent excess in all-cause mortality which reaches almost 20% at 5 years. This is partly due to a combination of underlying diseases that predispose to osteoporosis, and subsequent high-mortality fractures (for which vertebral fractures are a risk factor). Treatments for vertebral osteoporosis reduce fracture risk at all sites, but have not been shown to reduce mortality.
Nonvertebral fractures
The diagnosis of nonvertebral fractures is usually straightforward, although many doctors would admit to having missed a femoral neck fracture in a confused elderly person at least once. Most fractures present to medical attention promptly, but the importance of osteoporosis as a causal factor is still often overlooked. Although fractures of the distal radius and proximal femur are most clearly linked to bone fragility, virtually all fractures other than those of the facial bones and skull are markers of osteoporosis. As this is now well recognized, there are medicolegal implications for failing to investigate and treat appropriately after a first fracture.
Other presentations: risk factors and the worried well
Many conditions are associated with osteoporosis, and these are shown in Table 22.1. Most are detectable by taking a careful clinical history, and this is essential to the management of any patient with low-trauma fracture. By contrast, the diagnostic yield from physical examination is fairly limited. The general population is becoming much more aware of osteoporosis, partly through the excellent work of several nongovernmental organizations, and thus are requesting screening from their general practitioners. This should start with assessment of risk factors, and then further investigation should be offered if clinically justified, as bone density is just one component of risk; if it is not used in the context of other risk factors, much needless anxiety for the patient may result.
Figure 22.5 A dual-energy X-ray absorptiometry (DXA) scanner. With permission from Hologic, Inc.

Diagnosis
Plain X-rays
The role of plain radiography is to demonstrate the presence of a fracture. Osteoporosis is asymptomatic until fractures occur, so if a patient with back pain has no vertebral fractures on spine X-rays then the patient’s symptoms are not due to osteoporosis. Sometimes a working diagnosis of osteoporosis based on clinical history and fracture type is sufficient for managing the patient, but this is the exception. In some cases the possibility of osteoporosis may be suspected if plain radiographs show reduced contrast between bone and soft tissues. Abnormal bone texture may be apparent, and scoring systems such as the Singh grade have been used to assess bone fragility. However, in the absence of a fracture the predictive value of radiographic osteopenia is low unless other risk factors are present, and it should definitely not be regarded as synonymous with osteoporosis.
Bone mineral density measurement
Of the characteristics of bone that determine its strength, mineral content is the easiest to measure. Several techniques are available, with dual-energy X-ray absorptiometry (DXA) the best established (Figure 22.5). DXA uses two X-ray beams of different energies to image a region of interest such as the spine or hip, and then corrects for differences in soft-tissue attenuation to calculate BMD. DXA is the accepted standard for the WHO’s definition of osteoporosis in women (Figure 22.2). There is much evidence for the use of DXA to guide therapy for osteoporosis. However, very few drug trials have included patients over 75 years old, and none has related treatment efficacy to BMD measurement in this age group. Nonetheless, it seems reasonable to use BMD in the elderly as one important factor in deciding risk of fracture. Population screening for asymptomatic osteoporosis is not justified in the absence of proven treatments, and it is important to remember that a low BMD is only one risk factor for osteoporotic fracture.
Other radiological investigations
Other techniques for estimating bone strength include quantitative computed tomography (QCT) and various ultrasound-based devices. QCT is accurate and informative, but delivers a relatively high radiation dose, whereas ultrasound measurements involve no ionizing radiation but lower precision. Ultrasound techniques combine BMD with an ill-defined quality termed “bone stiffness”. The best predictor of fracture risk appears to be broadband ultrasound attenuation (BUA). This variable is a measure of the rate of change of ultrasonic attenuation with increasing frequency, and the relationship between BUA and the physical properties of bone is complex. Ultrasound measurement has been shown to predict fracture risk in postmenopausal women, but its use in other groups is unvalidated. Unfortunately, ultrasound machines are appearing increasingly in high-street shops for walk-in screening, where a false positive may produce much needless anxiety in healthy young subjects.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree