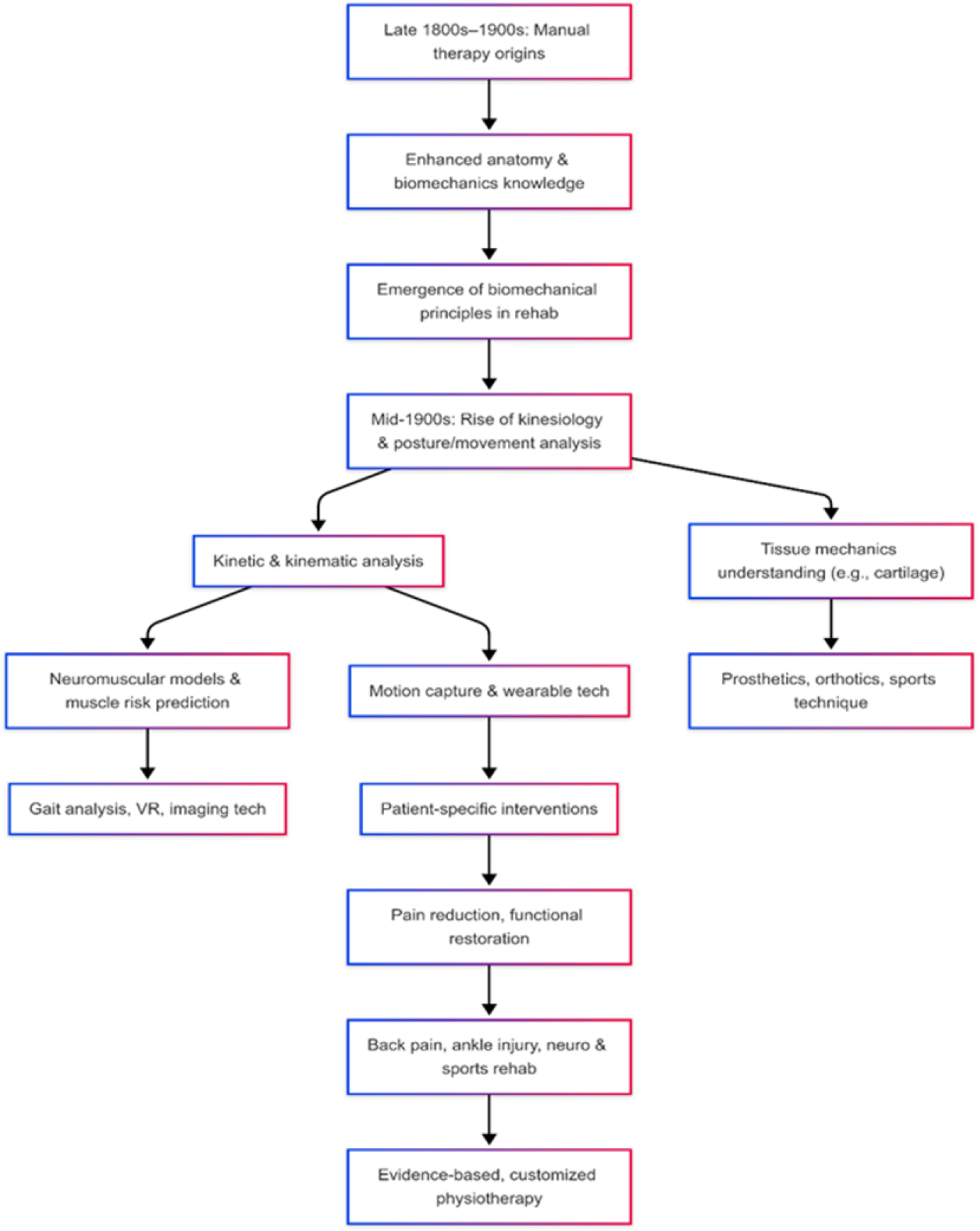
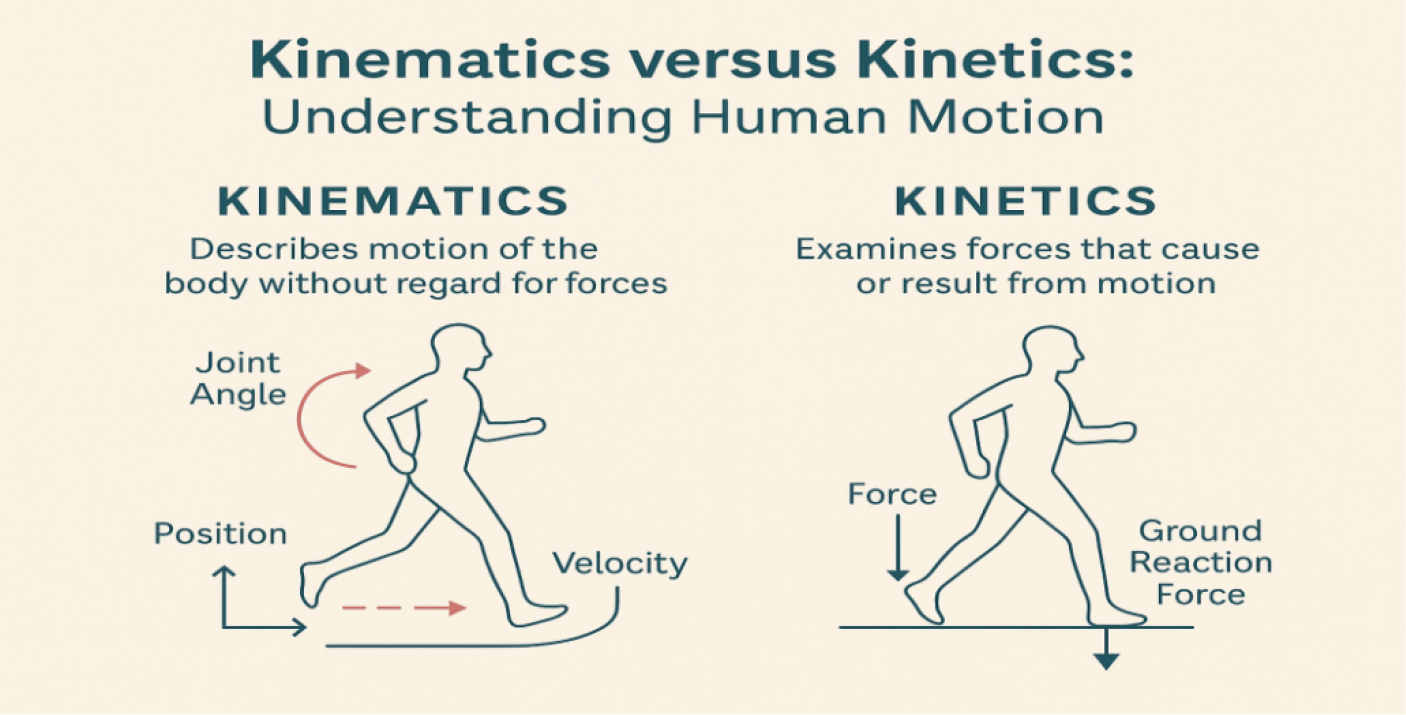
Biomechanics is an integral part of physiotherapy practice; it integrates the physics and engineering principles with clinical practice to optimize human movement analysis, injury rehabilitation and functional recovery. This review highlights various foundational biomechanical principles – kinematics, kinetics, tissue mechanics and neuromuscular control – and their potency in transforming evidence-based physiotherapy. Using state-of-the-art technology such as wearable sensors, motion-capture systems and machine learning methods, physiotherapists can now objectify movement patterns, calculate joint loadings and personalize rehabilitation programs to suit individual cases. Orthopedic rehabilitation, as well as neurological and sports rehabilitation, have all benefited from this approach, with results that are demonstrably better among patients suffering from ligament injuries, osteoarthritis and gait disorders induced by stroke. Despite these advancements, significant gaps remain; for instance, new types of exercises are not sufficiently included for pediatric and geriatric patients, there is insufficient solvable time in using robots for rehabilitation, and the mechanisms of tissue remodeling remain poorly understood. Progress against these challenges will require interdisciplinary collaboration and equitable access to biomechanical tools and evidence-guided interventions. For future directions, the use of artificial intelligence in predictive models and extending biomechanical treatment plans to medical areas with underserved patients should be emphasized. Combining technological innovation and clinical expertise, this review highlights the urgency of applying biomechanics to raise physiotherapy standards and improve care for patients. The history of biomechanics in physiotherapy began as early as the late 1800s and early 1900s when therapeutic intervention centered around hands-on techniques (i.e. mobilization, massage). Through an enhanced understanding of anatomy and biomechanics, biomechanical principles emerged as an important consideration for optimizing rehabilitation strategies (Kumar and Goyal 2024; Simplicio et al. 2024). This was the evolution of biomechanical principles into clinical practice, which in turn inspired more efficacious methods of treatment. Biomechanics is the science of the mechanical aspects of living organisms (see Figure 15.1). It uses the principles of physics and engineering relating to the human body system and analyzes forces, motion and musculoskeletal structures, with primary attention being paid to their role in movement and stability (Forte and Teixeira 2023; Tai et al. 2023). In physiotherapy, this discipline provides a fundamental framework to diagnose, treat and rehabilitate musculoskeletal disorders based on mechanical interactions in the body. Kinesiology made its mark as a discipline in the mid-20th century with the advent of kinesiological studies that became an important landmark in the development of kinesiology. These studies correlated posture, handling joints and movement patterns – the ground for therapeutic strategies including soft tissue mobilization and myofascial release, effective in pain diminishing and functional restoration (Cuesta‐Barriuso et al. 2021; Fereydounnia et al. 2022; Hryshyn and Antonova-Rafi 2023). This includes kinetic (forces on the motion) and kinematic (motion) analysis to help obtain performance, injury prevention and rehabilitation benefits (Donnelly et al. 2020; Tai et al. 2023). In healthcare, it is used to enhance prosthetics, orthotics and rehabilitation techniques, while in sports, it assists in technique improvement and injury avoidance (Donnelly et al. 2020; Tai et al. 2023). Tissue mechanical attributes, especially cartilage, underlie many joint functions and are the basis for therapeutic endeavors for disorders, including osteoarthritis (Alzahrani and Ullah 2024; Plakias et al. 2024). Neuromuscular models are designed to predict muscle activation and estimate muscle injury risks. Motion capture systems and wearable devices can monitor these interventions in real time (Alzahrani and Ullah 2024; Plakias et al. 2024). In particular, ground reaction forces data can be used to monitor recovery progress and provide valuable information on refined aspects of patient recovery (Sikorski and Czamara 2021). Biomechanically informed rehabilitation is effective for pain management, function and injury prevention. It is used in pediatric and geriatric populations, as well as in sports, fine-tuning treatment approaches dependent on individual musculoskeletal preferences (Loudon et al. 2011). Multiple studies indicate it to be more effective than traditional rehabilitation methods, particularly for back pain and ankle injuries (Miles and Mazdarani 2024; Saud murdef et al. 2024). The introduction of virtual reality and imaging technologies further allows for accurate patient-centered physiotherapy, with the use of targeted interventions (Grant and Mohtadi 2010; Bemani et al. 2021). Figure 15.1. Evolution of biomechanics in rehabilitation and physiotherapy Biomechanics is a critical aspect of modern physiotherapy, providing valuable insights into movement mechanics that help improve the quality of assessment and rehabilitation, and ultimately improve patient care. This review describes basic biomechanical principles, explores the supporting literature, reviews their application in clinical practice and education, identifies current gaps and outlines future directions This review retrieved biomechanical studies (foundational and applied) used in physiotherapy, selecting English-language sources encompassing peer-reviewed journals, textbooks, reports and grey literature. Data were obtained from PubMed, ScienceDirect, IEEE Xplore and the International Society of Biomechanics journals. Fundamental principles of biomechanics related to the fields of physiotherapy, sports science and medicine provide a guide to understanding human movement and guiding rehabilitation. The basic principles of Newton’s laws of motion describe how muscles and joints work together to provide stability and deal with external forces to prevent injuries and improve performance (Ortíz and Micheo 2011; Andrade‐Campos et al. 2012; Hamill et al. 2012; Brumitt et al. 2013; Hewett et al. 2017; Mustafy et al. 2019; Forte and Teixeira 2023). Stress–strain relationships and Wolff’s Law further define how tissue responds to mechanical loading, providing evidence towards strategizing inputs for orthopedic interventions and recovery methods (Ortíz and Micheo 2011; Andrade‐Campos et al. 2012; Brumitt et al. 2013; Mustafy et al. 2019). Biomechanics even extends to mechanotransduction on the cellular level, where mechanical cues lead to cellular responses, propelling applications in tissue engineering and regenerative medicine (Mistry et al. 2017; Wang and Galli 2018). Technological innovations (e.g. soft wearable electronics, inertial sensors and computational models) facilitate the enhancement of motion analysis and, in turn, clinical decision-making (Erdemir et al. 2018; Lu et al. 2024). Kinematics, which focuses on the parameters of motion, such as position, velocity and acceleration, contributes to diagnosing motor dysfunctions and developing rehabilitation programs, which are especially relevant in the context of virtual reality and inertial measurement systems (Tulipani et al. 2018; Hua et al. 2020; Yogesh et al. 2023; Guo et al. 2024; Zhou and Guo 2024). Kinetics, in contrast, examines forces that affect motion – torque and equilibrium – that underlie joint stability and balance. Kinematics and kinetics are the two major components in biomechanics that need to be understood to understand human motion (see Figure 15.2). Kinematics is the physics of motion, including quantities such as displacement, velocity, acceleration and joint angles. Kinematic analysis is particularly useful for evaluating the mechanics of movement, detecting gait impairments and monitoring rehabilitation progress (Czamara et al. 2015). Figure 15.2. Kinematics versus kinetics: understanding human motion In contrast, kinetics studies the internal and external forces acting on the body, such as the muscle forces, joint torques and ground reaction forces. This is important for the knowledge of joint loading, designing training protocols (Twumasi 2025) and avoiding overuse injuries. The combined analysis of kinematic and kinetic data is always helpful to understand the movement science and direct intervention for diagnosis and rehabilitation (Orishimo et al. 2010; Sikorski and Czamara 2021). Functional movement screening is an example of a tool operating from a model similar to that of health and disease, using both types of data to identify compensatory patterns and evaluate the likelihood of injury in a population, with the aim of establishing individualized and effective rehabilitation protocols (Pan et al. 2011). Refinements in motion capture systems and wearable inertial sensors have improved the usefulness of these for clinical practice. These instruments acquire real-time, objective data on joint motion and symmetry that contribute to clinical decision-making, particularly in the field of stroke rehabilitation (García 2022; Lee et al. 2022; LeMoyne and Mastroianni 2023). Kinematic and kinetic gait assessment provides a more complete understanding of motor control in health and disease (Lyu et al. 2021; Hui and Song 2023). The kinetic chain model supports a system-based approach to understanding how joints and muscles work together, again emphasizing the need to consider the entire body in rehabilitation.Table 15.2 and Figure 15.2 summarize the structure of the developed framework to present an all-encompassing view of human movement that can contribute to the industry of clinical practice and sports performance optimization. The reliance on the common motor framework means disruptions in one region can affect the whole system, which, in turn, highlights the importance of task-specific training and functional exercises that imitate real-life activities (Ličen et al. 2021; Brückner et al. 2023; Kim et al. 2023). Novel technologies, such as robotic-assisted rehabilitation, enable accurate motion guidance and simultaneously collect real-time kinematic data, enhancing movement precision and therapeutic regularity (Lyu et al. 2021; Patel et al. 2021; Ceglia et al. 2023). Machine learning combined with kinetic analysis has also shown predictive ability for rehabilitation, opening a new frontier of data-driven personalized care (Halilaj et al. 2018; Shanshan et al. 2018). Medical rehabilitation practitioners can thus use assessments that include aspects of both kinematics and kinetics, which have been proven to improve functional gains in patients. Table 15.1. Kinetics versus kinematics Physiotherapy and rehabilitation are closely tied with biomechanical concepts such as the planes of movement, axes of rotation, lever systems and types of muscle contractions and so on, and these concepts are the most fundamental for clinicians, as they provide the base in terms of movement analysis, design of individualized rehabilitation protocol and finally enhancing the functional outcomes for patients with a plethora of musculoskeletal and neurological conditions. It is summarized in Table 15.2. Table 15.2. Planes and axes of movement The body functions as a system of levers, enabling efficient force generation and movement. These levers are categorized into: Center of gravity (CoG) and balance mechanics are important in physical rehabilitation, not only for the treatment of injuries but also in managing chronic conditions. The location of the CoG, which is where most of the body mass is focused, influences the balance control during dynamic and stationary tasks. Balance depends on proper CoG alignment relative to the base of support. CoG mechanics are of particular interest in rehabilitation, where therapies often aim to improve balance and minimize the risk of falls. Balance training aids in CoG alignment and strength training (Mkacher et al. 2015). Segmental assessment of trunk alignment during balance activity, particularly in a virtual reality environment, enhances stability (Feng et al. 2019) in individuals with Parkinson’s disease. Wobble boards, commonly used in rehabilitation programs, specifically for older adults, focus on stimulating the CoG and proprioception, facilitating balance (Ogaya et al. 2011). Comprehensive balance training following hip fractures improves postural stability and lowers fall rates (Chang et al. 2024). Balance control is a complex process that requires adequate muscle strength, neuromuscular coordination, dynamics and interaction with our environment. The vestibular system is also trained and strengthened, while the muscle strength improves to manage CoG over Base of Support (BoS) (Mkacher et al. 2015). Modern technologies, including biofeedback and wearable sensors, have made it possible to visualize dynamic changes in CoG in real time, as patients posturally adjust to achieve improved functional balance (Sadura-Sieklucka et al. 2023; Museck et al. 2024). These are especially beneficial for at-risk populations, as they have a higher risk of falling while they recover. Biomechanics is an important component of almost all aspects of clinical practice in physiotherapy. The systematic and evidence-based approach provided by biomechanics – brings an improved understanding of human body movement and a greater appreciation for how this understanding can be harnessed to improve clinical outcomes. It is summarized in Table 15.3. Table 15.3. Clinical applications of biomechanics in physiotherapy Biomechanics is regularly used in clinical practice, rehabilitation and injury prevention, providing important insights into tissue properties, movement patterns and injury mechanisms (see Figure 15.3). Through biomechanics, identification of movement and dysfunctions from clinical assessment to evaluation biomechanics provides the toolbox to understand applied mechanical forces acting on the body from daily activities. An example of this is the general gait analysis, a standard technique used to assess various joint kinematics, muscle activity and movement strategies, and identify functional limitations, provide fall risk evaluation in elderly subjects or support postoperative rehabilitation (Hausdorff et al. 2001; Perry and Burnfield 2010). Clinicians can identify compensatory movement patterns, asymmetries and dysfunctional postures in people with cerebral palsy, Parkinson’s disease and stroke by using kinematic and kinetic analyses (Winter 2009
15
Biomechanics in Physiotherapy
15.1. Introduction
15.2. Methodology
15.3. Literature review
15.3.1. Basic biomechanics principles
15.3.2. The core biomechanical principles
15.3.2.1. Kinematics versus kinetics
Aspect
Kinetics
Kinematics
Definition
Studies the forces and torques that cause motion in objects
Describes the motion of objects without considering the forces causing the motion
Focus
Analyzes the causes of motion, including forces and torques
Examines the motion itself, focusing on parameters such as displacement, velocity and acceleration
Consideration of mass
Mass is a crucial factor; it influences how forces affect motion
Mass is not considered; the study is independent of the object’s mass
Involvement of forces
Directly involves forces; it seeks to understand how forces result in motion
Does not involve forces; it describes how objects move regardless of the forces acting upon them
Applications
Used to analyze joint loading, design strength training and prevent overuse injuries (Twumasi 2025)
Used to assess joint movement patterns, detect gait abnormalities and track recovery progress after surgeries
Example
Analyzing the forces acting on a car to determine its acceleration
Calculating the trajectory of a projectile without considering air resistance or other forces
15.3.2.2. Planes, axes, levers and muscle contraction
Plane
Axis
Movements
Rehab focus
Sagittal
Frontal
Flexion, extension
Knee/hip/shoulder/elbow/ wrist rehab, ROM recovery (Gökşen et al. 2021; Abudouaini et al. 2023; Hou 2023)
Frontal
Sagittal
Abduction, adduction
Knee/hip rehab, ROM recovery (Gailey et al. 2020)
Transverse
Vertical
Rotation, IR/ER
Core stability, coordination (Highsmith et al. 2016a, 2016b)
15.3.2.3. Lever systems in the body
15.3.2.4. Center of gravity and balance
15.3.2.5. Balance training benefits in CoG alignment and muscle strength and Chronic Obstructive Pulmonary Disease (COPD)
15.3.3. Biomechanics in clinical practice
Application area
Biomechanical focus
Clinical benefits
Assessment
Gait analysis, joint kinematics and muscle activity
Identifies functional impairments, assesses fall risk and guides postoperative recovery (Hausdorff et al. 2001; Perry and Burnfield 2010)
Rehabilitation
Injury mechanism analysis, personalized exercise programs, prosthetics and orthotics design
Enhances recovery outcomes, reduces reinjury risk and improves movement efficiency (Milanesi et al. 2017; Hughes et al. 2020; Uchida et al. 2023)
Injury prevention
Movement pattern analysis, neuromuscular training and ergonomic assessments
Identifies injury risks, develops targeted prevention strategies and enhances athletic performance (Woo et al. 2006; Nigg and Benno 2007; Padua et al. 2009; Winter 2009; Hewett et al. 2017)
Manual therapy
Joint biomechanics, mobilization force vectors and tissue tension assessment
Improves manipulation precision, reduces pain and enhances ROM (Pasquier et al. 2022; Lee and Kim 2023)
Movement analysis
3D kinematics, force plate analysis and EMG integration
Identifies movement dysfunctions and enhances therapy planning (Hegedus et al. 2011; Tatsios et al. 2022).
Musculoskeletal
Tendon and ligament mechanics, spinal alignment and load-bearing patterns
Improves diagnosis, guides surgical/rehab decisions and reduces load-related pathologies (Haan et al. 2011; Çetin et al. 2019; González-Pola et al. 2021; Panda et al. 2022; Bali et al. 2023; Silvestros et al. 2024)
Neuromuscular control
Motor unit coordination, proprioceptive feedback and neuromechanics of reflexes
Refines balance training, supports stroke rehab and aids motor recovery (Dutta et al. 2014; Danielson et al. 2023; Jouira et al. 2024)
Cardiopulmonary
Chest wall expansion mechanics, diaphragm movement and vascular compliance
Improves respiratory training and monitors circulatory strain during rehab (Albarrati et al. 2018; Holzapfel and Ogden 2018; Gregory et al. 2022)
Integumentary
Pressure distribution analysis, shear force quantification and tissue stress
Aids ulcer prevention and supports seating/positioning interventions (Everett and Sommers 2012; Gill 2015; Wahyuni et al. 2023)
Sports rehabilitation
Kinematic efficiency, jump landing mechanics, agility and coordination assessment
Boosts performance, decreases risk of reinjury and optimizes return-to- sport protocols (Healy et al. 2019; Bali et al. 2023; Brazuna et al. 2023)
15.3.4. Applications in assessment, rehabilitation and injury prevention
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree



