Introduction
Before initiating the laboratory workup of any patient with a suspected defect of hemostasis, the hematologist must first verify that the patient has a clinical history, signs, and symptoms compatible with a bleeding disorder. This is not an easy task because mild bleeding and bruising are common in the general population. Furthermore, bleeding, particularly in the outpatient setting, is difficult to quantify because patient reports may be biased; the definition of “excessive” bleeding or bruising is subjective and varies among individuals. Additionally, a critical consideration in children is the fact that many of them have not had specific hemostatic challenges such as surgeries or menarche that might unveil a bleeding disorder. All these factors contribute to the difficulty in the diagnosis of bleeding in the pediatric population.
Therefore, an accurate diagnosis is made primarily by obtaining a thorough personal and family history and then performing a careful physical examination, which will lead to an appropriate set of laboratory tests. Once suspicion for a bleeding disorder is confirmed, the remaining workup items are implemented in a focused manner with reference to particular differential diagnoses.
Children with suspected bleeding disorders might present for evaluation in a variety of ways: concerning signs and symptoms, abnormal presurgical screening laboratory results, or a known family history of hemostasis defects that requires consultation. The variety in severity of different bleeding disorders also results in children presenting at different ages. The goal for the consulting hematologist is to approach the child with a broad differential diagnosis in mind, narrow the options by carefully assessing the medical and family history as well as pertinent physical findings, and order the most appropriate laboratory tests to reach a diagnosis and initiate definitive therapy, if indicated.
Although the approach to the bleeding child is often similar in the outpatient and inpatient setting, the practicing hematologist is sometimes consulted because of bleeding in the critically ill patient. In such cases therapeutic measures will likely be required immediately and an accurate diagnosis made later.
Clinical Evaluation
The initial clinical evaluation of a child with a suspected bleeding disorder starts with a series of questions, usually at a doctor’s office or clinic, that attempt to summarize the most important aspects of the clinical presentation and history of bleeding. Although several standardized bleeding assessment tools have been used recently in research projects, their value in clinical practice is still unproven. Therefore, questions should be designed to establish certain parameters that would prompt an appropriate laboratory workup. The initial set of questions should establish the following: (1) the most common site and type of bleeding (e.g., mucocutaneous versus articular or deep muscle), (2) bleeding on hemostatic challenge such as surgeries or trauma, and (3) family history of bleeding.
Clinical Presentation of Bleeding
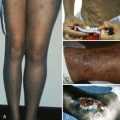
Significant surgical or postoperative hemorrhage, rectal or genitourinary bleeding, and major muscle or joint bleeding are easily identified as abnormal, but they represent a minority of new cases. Most often the clinician’s challenge consists in differentiating mild but common presenting symptoms of bleeding disorders, such as easy bruising and mucosal bleeding (e.g., epistaxis, menorrhagia, oropharyngeal), from those encountered in healthy children and then determining when additional laboratory evaluation is warranted. Large bruises without previous significant trauma, disseminated petechiae, intramuscular hematomas, hemarthrosis (joint effusion, warmth, and pain with passive movement) usually indicate a bleeding disorder. In young children, refusal to walk is often a sign for an extremity-related bleed and could represent the first sign of hemarthrosis in a boy with hemophilia ( Table 29-1 ).
| Clinical Characteristic | Primary Hemostatic Defect | Clotting Factor Deficiency |
|---|---|---|
| Site of bleeding | Skin, mucous membranes | Soft tissues, muscles, joints |
| Bleeding after minor cuts | Yes | Rare |
| Petechiae | Present | Absent |
| Ecchymosis | Small, superficial | Large, deep, palpable |
| Hemarthrosis | Rare | Common |
| Bleeding after trauma/surgery | Immediate | Delayed |
Susceptibility to increased bruising must first be differentiated from nonmedical causes such as abuse, a phenomenon that is, unfortunately, common enough to warrant its own set of guidelines for evaluation in recent reports from the American Academy of Pediatrics. Inflicted trauma is most likely to manifest over the head, chest, back, and long bones (and may retain the outlines of the instrument used to inflict harm), whereas bruises associated with primary hemostasis defects are usually located over areas of typical childhood trauma, such as bony protuberances of extremities or spinous processes.
Epistaxis is a frequent presenting sign in children with hemostatic disorders, but it is also a common complaint among healthy children, usually the result of local aggravating factors (dry nasal mucosa, trauma, allergic rhinitis). In a recent study of 248 children referred to the otolaryngology clinic at Children’s Hospital of Philadelphia for epistaxis, 11% were found to have a bleeding disorder (type 1 von Willebrand disease [VWD], platelet aggregation defect, or mild factor VII deficiency), with clinical predictive factors being younger age or previous emergency medical care for the epistaxis. Other studies, however, have found an incidence as high as 25% to 33% for coagulopathy among children referred to pediatric hematologists for recurrent epistaxis. Therefore it is important that epistaxis be taken seriously as a presenting symptom, particularly in cases that require emergency medical care, occur in both nostrils, or appear in association with other bleeding signs or a family history of similar bleeding.
Menorrhagia is also a frequent presenting sign for mild or moderate bleeding disorders (including VWD, platelet function disorders, and other coagulopathies) and can quickly lead to severe anemia and decreased quality of life. The classic definition of menorrhagia (i.e., greater than 80 mL of blood loss per cycle) is rarely used clinically because most women describe limitations of their daily activities as more important than the actual volume of blood lost. A more popular working definition is “excessive cyclic uterine bleeding that occurs at regular intervals over several cycles, or prolonged bleeding that lasts for more than 7 days”. In fact, the American College of Obstetrics and Gynecology has recommended that testing for VWD be performed in all adolescents with severe menorrhagia, although a subsequent meta-analysis determined that there may not be adequate data to support this universal recommendation. It is essential for practitioners to be judicious about laboratory testing in adolescents with menorrhagia. All adolescents that present with menorrhagia should be evaluated by a gynecologist; testing for a bleeding disorder is not always warranted, particularly in the absence of family and personal history or other bleeding manifestations.
Surgical (e.g., circumcision, tonsillectomy) or dental (e.g., extractions) bleeding also may be associated with disorders of hemostasis. This type usually manifests as uncontrolled bleeding during or after the procedure, bleeding that extends beyond the surgical site, unexpected need for blood transfusion, or delayed bleeding after a procedure.
Hereditary hemorrhagic telangiectasia may also be manifested as mucosal bleeding, particularly epistaxis. Profuse bleeding into soft tissues or joints suggests deficiency of a coagulation factor (such as factors VIII or IX). Umbilical stump bleeding is typically seen with factor XIII deficiency, but it may also occur with deficiencies of prothrombin, factor X, and fibrinogen.
After establishing the possibility of a true bleeding disorder, the clinician should next consider a broad differential diagnosis for the bleeding child and approach the history taking and physical examination with the intent to systematically remove options and pare down the list to a certain category or group of potential diseases. Briefly, the main categories to be considered should include anatomic abnormalities, quantitative and qualitative platelet defects affecting platelet plug formation (primary hemostasis), and quantitative and qualitative defects of clot propagation (secondary hemostasis). Differentiation also must be made between inherited and acquired disorders. Common diseases should be considered before rare ones, and diagnoses that are either life threatening or easy to treat should be prioritized in the evaluation process.
Finally, it is clear that the clinical assessment and the laboratory workup of the bleeding child will vary depending on the emergent nature of the clinical situation. The practicing hematologist is often consulted in the inpatient setting regarding bleeding in the intensive care unit or operating room. The approach in these situations is sometimes limited by the inability to obtain reliable baseline hemostatic laboratory values because of the presence of active disease or the fact that most patients receive hemostatic agents (including blood products) to stop the hemorrhage. Therefore it becomes difficult to distinguish congenital bleeding conditions frin acquired ones. Often the immediate need for treatment supersedes a more thorough evaluation. In these cases it is reasonable to treat the patient and then, if a baseline defect of hemostasis is suspected, perform the laboratory evaluation days or even months after the episode, when the acute process is resolved.
Relevant Clinical History
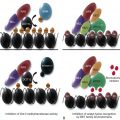
Information about the patient’s previous response to hemostatic challenges (e.g., surgical procedures, invasive dental work, traumatic injuries) is an essential part of the initial evaluation. For example, a congenital hemorrhagic disorder is unlikely in a patient with a history of surgical procedures or tooth extractions without any abnormal bleeding, whereas postoperative transfusion requirements and iron-responsive anemia often signal hemostatic defects. In view of the variability of patients’ perception of bleeding, as well as the lack of a uniform clinical measure of bleeding severity, the history may be most discriminatory when a standardized and validated questionnaire is used and a “bleeding score” is incorporated into the diagnosis. Several such instruments currently exist, but consensus on a single questionnaire that can quantitate bleeding optimally is still evolving. The International Society of Thrombosis and Hemostasis (ISTH) Joint Scientific Subcommittee (SSC) on von Willebrand factor (VWF) and Pediatric/Perinatal Bleeding Disorders recently developed a bleeding assessment tool to provide more accurate determination of bleeding phenotype in individuals with bleeding disorders and compared them to healthy subjects. The main objective of all the existing bleeding assessment tools is to accurately diagnose bleeding and predict the risk of bleeding in the future. However, owing to their high negative predictive value, it is becoming increasingly clear that these new instruments are more effective at excluding the likelihood of a bleeding disorder than predicting future bleeding risk. Family history is also a key component in establishing both the likelihood of an inherited bleeding disorder and its specific nature. However, determination of which family members may have been affected by relying on testimony from one or more relatives can be difficult. Therefore the ISTH SSC on VWF has a specific definition of a positive family history for VWD. In summary, a personal history of bleeding triggers clinical and laboratory evaluation, and a positive family history serves as supportive evidence for a hereditary bleeding disorder.
The history of the present illness often provides useful clues to the diagnosis, including several classic types of presentation. A sick child with fever, shock, and mucocutaneous purpura may have disseminated intravascular coagulation (DIC) associated with bacteremia. Hemophilia should be considered in a male toddler who has just started crawling and exhibits subcutaneous or joint bleeding, or who bleeds after circumcision. A girl who has had severe menorrhagia since menarche may have VWD. A well-appearing child covered with petechiae likely has immune thrombocytopenia, but if the lesions are localized to the buttocks, ankles, and feet, and they present as palpable bruises, Henoch-Schönlein purpura should be considered.
When applicable, a detailed menstrual history, including age at menarche, duration of menses, interval between menses, and frequency of pad or tampon replacement necessary to control the bleeding, should be obtained. The prevalence of bleeding disorders in women with menorrhagia is as high as 20%, and menorrhagia is a common initial symptom in women with VWD (approximately 90% of female patients).
It is also important to note whether the patient has an underlying medical disorder that may affect hemostasis, such as hepatic or renal disease, malabsorption syndrome, or Ehlers-Danlos syndrome (EDS) or another connective tissue disorder. Most of the coagulation proteins are synthesized in the liver, and as a result, liver insufficiency is a common cause of prolongation of clotting times and bleeding. Certain metabolites that accumulate in uremia can interfere with platelet function, whereas low-molecular-weight coagulation proteins (factors IX and XI) are lost through the kidney in children with nephrotic syndrome. In malabsorption syndrome, levels of the vitamin K–dependent coagulation factors (II, VII, IX, and X) may be depleted and lead to excessive bleeding. A child with cyanotic congenital heart disease and polycythemia may have petechiae and excessive bleeding with surgery, in part as a result of thrombocytopenia, hypofibrinogenemia, or both.
Age of Onset
It is also important to investigate the age of onset of clinical bleeding. Generally, early age of onset correlates with more severe bleeding and may indicate a congenital cause. Bleeding that develops later in childhood may indicate either an acquired problem or a milder congenital bleeding disorder. For example, mild hemophilia may not be diagnosed until late childhood or adolescence, when participation in contact sports presents an increased hemostatic challenge. Postcircumcision hemorrhage, umbilical stump bleeding, cephalohematomas, and subgaleal hemorrhage are cardinal manifestations of underlying bleeding disorders and should be evaluated thoroughly. The incidence of neonatal intracranial hemorrhage among boys with hemophilia is estimated to be as high as 3% and may be as high as 25% in patients with FXIII deficiency.
The neonatal period (first 4 weeks after delivery) is a time of unique transitional physiology, which includes the coagulation system. The neonate has physiologically decreased levels of most procoagulant and anticoagulant proteins (although levels of acute phase reactants, such as factor VIII and fibrinogen, are normal), and thus the hemostatic system can be easily overwhelmed, potentially during the significant head trauma associated with labor and vaginal delivery. One study reported intracranial hemorrhage (ICH) after spontaneous vaginal delivery at a rate of 1 per 1900, whereas the rate of ICH in babies delivered by vacuum-assisted delivery was 1 in 860. In addition, 15% to 30% of patients with inherited bleeding disorders have bleeding manifestations in the neonatal period, and certain disorders, such as neonatal alloimmune thrombocytopenia (NAIT), are unique to the neonatal period. Furthermore, the neonate is significantly affected by the state of maternal health and medications used during labor. Because of the small blood volume in a neonate, a relatively small degree of blood loss can have major hemodynamic consequences.
When evaluating bleeding in a neonate, the hematologist must first assess whether the baby is healthy or has medical conditions that may have precipitated hemorrhage. It is important to inquire about prolonged rupture of membranes, chorioamnionitis, and fetal distress during labor. Additional details about the mother’s state of health, including infections, autoimmune disease, and platelet count, should be obtained. Vitamin K administration to the baby should be confirmed. The neonate should be examined, with particular attention directed to the presence of birth trauma, bruises, and petechiae and evidence of flank masses (renal vein thrombosis), which can cause thrombocytopenia. The presence of hepatosplenomegaly may suggest disseminated intrauterine infection. When blood is obtained for various coagulation tests, particular attention should be paid to the patient’s hematocrit concentration and the volume of the sample. Additionally, all laboratory results should be compared with normal values for different gestational ages.
Isolated thrombocytopenia in a healthy infant may be seen in NAIT, in maternal autoimmune thrombocytopenia, or in cases of decreased platelet production such as amegakaryocytic thrombocytopenia or the syndrome of thrombocytopenia with absent radii. Rarely, type 2B VWD may be manifested as thrombocytopenia in a well infant. Thrombocytopenia in sick neonates is often due to the underlying cause, such as infection or DIC. Isolated prolongation of the prothrombin time (PT) or activated partial thromboplastin time (APTT) in a healthy baby may be caused by a specific clotting factor deficiency in the extrinsic or intrinsic pathway, respectively, and prolongation of both the PT and APTT suggests either a common pathway clotting factor deficiency or vitamin K deficiency (hemorrhagic disease of the newborn). The so-called early vitamin K deficiency–associated bleeding usually presents in the first week of life and is associated with nutritional deficiencies or failure to administer vitamin K at birth, whereas late vitamin K deficiency bleeding occurs between 3 and 8 weeks after birth and may manifest as intracranial hemorrhage or severe gastrointestinal bleeding.
Family Bleeding History
The family history is essential for assessing differential diagnoses. The hematologist should inquire about any known or suspected bleeding problems in other family members, including any specific diagnoses. If the family history is positive for bleeding, the hematologist should note the type and severity of bleeding (e.g., joint bleeding, epistaxis, menorrhagia), age at onset, and the relationship of the affected family member or members to the patient. An X-linked recessive inheritance pattern (maternal cousins, uncles, and grandfather) suggests a diagnosis of hemophilia A or B, whereas an autosomal dominant pattern would be more consistent with VWD or hereditary hemorrhagic telangiectasia. Most other clinically relevant clotting factor deficiencies are inherited in an autosomal recessive manner, and the family history is frequently negative for bleeding, although consanguinity may be noted.
Approximately one third of infants and young children with newly diagnosed hemophilia have a negative family history, consistent with the Haldane hypothesis for the fraction of new mutations in all lethal X-linked recessive disorders. For VWD, considerable variation in symptoms may be noted among affected family members because of the incomplete penetrance (i.e., not every person that inherits the mutation will exhibit an abnormal phenotype) and variable expressivity (i.e., family members with the same mutation have a variable phenotype) that are hallmarks of this disease. Bleeding manifestations may be very mild in some and give the misleading impression of a negative family history. Factor XI deficiency, an autosomal trait most often (but not exclusively) seen in persons of Ashkenazi Jewish descent, may be associated with a very mild or moderate tendency for bleeding. The degree of bleeding manifestations does not correlate well with the level of factor XI or the APTT, although the patient’s specific mutation may be predictive.
Medications
A careful history of medication use should be obtained, including prescribed medications, over-the-counter drugs, recreational drugs, and herbal products. A number of drugs are associated with bleeding diatheses, with mechanisms including induction of thrombocytopenia (e.g., quinine or quinidine, rifampin, trimethoprim-sulfamethoxazole, carbamazepine, cimetidine, ranitidine, valproic acid) and platelet dysfunction (nonsteroidal antiinflammatory drugs [NSAIDs] such as ibuprofen [reversible effect] and aspirin [irreversible]). In the case of medications that cause platelet dysfunction, it is important to note that they primarily exacerbate preexisting bleeding disorders rather than cause clinically relevant bleeding by themselves. In addition, prolonged antibiotic use may lead to lower vitamin K levels and induce bleeding secondary to acquired deficiency of vitamin K–dependent factors. Table 29-2 lists medications, compounds, and herbal supplements known to be associated with bleeding.
| Effect | Compound Class | Examples | Mechanism |
|---|---|---|---|
| Platelet dysfunction | COX-1 inhibitors | Aspirin, ibuprofen, naproxen | Inhibit conversion of AA to thromboxane A2 |
| Thienopyridines | Clopidogrel, prasugrel, ticagrelor, cangrelor | Inhibit ADP-induced platelet activation | |
| Phosphodiesterase inhibitors | Dipyridamole, cilostazol | Increased cAMP decreases agonist-induced activation | |
| GPIIb/IIIa inhibitors | Abciximab, tirofiban, eptifibatide | Inhibit integrin activation and conformational change | |
| β-Lactam antibiotics | Cephalosporins, penicillins (esp. in high doses) | Inhibit epinephrine- and ADP-induced aggregation and granule release. Also, interference with platelet-VWF interaction | |
| SSRIs | Fluoxetine, olanzapine, citalopram, sertraline, escitalopram | Decrease platelet serotonin | |
| Herbs and foods | Ginkgo (Ginkgo biloba) Garlic (Allium sativum) Bilberry (Vaccinium myrtillus) Ginger (Zingiber officinale) Dong quai (Angelica sinensis) Feverfew (Tanacetum parthenium) Asian ginseng (Panax ginseng) American ginseng (Panax quinquefolius) Siberian ginseng/eleuthero (Eleutherococcus senticosus) Turmeric (Curcuma longa) Meadowsweet (Filipendula ulmaria) Willow (Salix alba) Black tree fungus (Auricularia polytricha) | Various | |
| Alcohol | Alcohol | Decrease P-selectin exposure | |
| Other | Amitriptyline, imipramine, chlorpromazine, cocaine, lidocaine, isoproterenol propranolol, penicillin, ampicillin, cephalothin, promethazine, diphenhydramine, carbenicillin | Interfere with platelet membrane | |
| Furosemide, verapamil, hydralazine, cyclosporine, hydrocortisone | Inhibit prostaglandin pathways | ||
| Caffeine, dipyridamole, aminophylline, theophylline, vinblastine, vincristine, colchicine, papaverine | Inhibit platelet phosphodiesterase | ||
| Thrombocytopenia | Antiepileptic drugs | Phenytoin, valproate, carbamazepine | Unclear |
| Glycoprotein IIB/IIIa inhibitors | Abciximab | Drug-dependent antibody | |
| Anticoagulants | Unfractionated heparin (more common) low-molecular-weight heparin (less common) | Drug-dependent antibody | |
| Foods | Quinine, white lupin, tahini, jui herbal tea | Various |
Physical Examination
A thorough physical examination must begin with an evaluation of the vital signs, with particular emphasis on potential signs of severe bleeding-related anemia or intravascular volume loss, such as tachycardia (early finding) or hypotension (late finding). Next, a global overview should be undertaken to observe the pattern of bleeding stigmata. Petechiae are small capillary hemorrhages and characteristically develop in crops in areas of increased venous pressure, such as dependent parts of the body or those compressed by elastic waistbands, sock tops, or straps (e.g., from backpacks, purses, luggage). They are painless, nonpalpable, and nonblanching and must be distinguished from small telangiectases and angiomas. In general, the presence of petechiae indicates a defect in primary hemostasis (platelet number or function or vascular integrity). Ecchymoses are palpable purplish lesions induced by subcutaneous bleeding and usually indicate a defect in secondary hemostasis (clot propagation), such as deficiency of a coagulation factor. Additionally, hemarthrosis, associated with severe coagulation factor deficiency, should be evaluated for joint size, swelling, and range of motion limitations. Identification of hepatomegaly and splenic enlargement may point toward coagulopathy associated with systemic disorders such as leukemia or hepatocellular disease.
Knowledge of the bleeding manifestations of certain syndromes can help the hematologist efficiently evaluate children with known syndromes. Conversely, the hematologist’s identification of a particular bleeding pattern may pave the way to an important syndrome diagnosis that can guide other system-based evaluation or interventions earlier than would otherwise be possible. For example, it is important for the hematologist to know that patients with Noonan syndrome can have thrombocytopenia, platelet function defects, and prolonged APTTs secondary to abnormalities of the intrinsic pathway (deficiencies of FVIII, FIX, FXI). Another example is the importance of recognizing bleeding related to skin or vascular fragility as a potential manifestation of heritable connective tissue disorders such as EDS. The molecular basis for bleeding in these syndromes is not well understood, but the clinical association between these syndromes and excessive hemorrhage is strong enough to warrant a careful investigation.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree