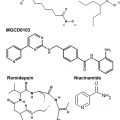
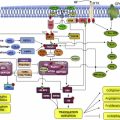
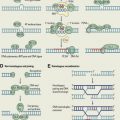
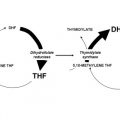
Of the agents available in the treatment of both solid and hematologic cancers, microtubule-targeted agents are among the most widely used and exploiting other mechanisms involving the microtubule and its role in mitosis is an area of continued interest. This review will focus on novel microtubule-targeted agents, both recently approved (eg, ixabepilone and eribulin) and in later-stage clinical trials, and kinase inhibitors that aim to directly inhibit the mitotic spindle, such as the aurora kinase, pololike kinase, and kinsein-spindle protein inhibitors.
- •
Microtubulin stabilizers have an important and established role in the treatment of solid tumors.
- •
Novel agents that approach the mitotics spindle are undergoing evaluation. These agents include aurora kinase inhibitors, kinesin spindle inhibitors, and pololike kinase inhibitors.
- •
Novel cytotoxics that are directed against the microtubular apparatus (eribulin and ixabepilone) have been approved for use in metastatic breast cancer.
In the last several years, research dedicated to carcinogenesis has focused on the therapeutic exploitation of signal transduction pathways. Among these, a classic and attractive target for the development of antineoplastic agents is centered on the basic backbone of the cell: the cytoskeleton.
Microtubules are integral components of the cytoskeleton. They function in multiple capacities (ie, in the maintenance of cell shape and polarity, intracellular transport, and in the formation and dynamics of the mitotic spindle). They represent a validated target for cytotoxic agents. In addition to modulators of microtubule dynamics, a body of literature shows the pivotal and integrative role of both tubulin-binding and nontubulin-binding agents. The kinesinlike proteins and the mitotic kinesins play a critical role in function of the mitotic spindle, chromosome segregation, mitotic checkpoint control, and cytokinesis, and represent druggable protein targets.
This article reviews the development of novel antimitotic targets and their small molecules.
Microtubule structure
Microtubules are hollow filaments that result from the polymerization α-tubulin and β-tubulin. They consist of a parallel arrangement of 13 protofilaments arranged in a head to tail order. One end is composed of α-tubulin (negative end) and the other end of β-tubulin (positive end), resulting in a polarized helix. Microtubules are anchored at the negative end to a network of microtubule-associated proteins, leaving the positive end disposed to the cell periphery. As a result of noncovalent association and disassociation of α and β heterodimers, microtubules oscillate between a state of polymerization and depolymerization. Two behaviors are shown by the microtubules: dynamic instability and treadmilling, both of which are dependent on the state of guanosine triphosphate (GTP). Dynamic instability refers to switching of microtubules between periods of slow growth and rapid shortening, whereas treadmilling is characterized by the net addition of a tubulin subunit to the positive end and the parallel loss at the negative end.
This engineered dynamic process is vital for the proper spindle function and subsequent alignment and segregation of chromosomes. Disruption of this process results in aberrant mitosis and prevents cell cycle progression, resulting in cell death.
Microtubule-targeting agents
Microtubule-targeting agents either inhibit microtubule polymerization, resulting in decreased microtubule polymer mass, or promote microtubule polymerization, resulting in increased microtubule polymer mass and stabilization. These compounds are characterized either as microtubule-stabilizing agents such as the taxanes and the epothilones or microtubule-destabilizing agents such as the vinca alkaloids and colchicines.
Microtubule-targeting agents bind to distinct binding sites on the β-tubulin. The vinca domain is located adjacent to the GTP binding site in the β-tubulin. The taxane site is located within the hydrophobic pocket between adjacent protofilaments in the lumen of the microtubule, whereas the colchicine site is located at the intradimer interface between the α- and β-tubulin.
The oldest classes of cytotoxic agents that interfere with microtubules are the vinca alkaloids. These agents (vincristine, vinblastine, vindesine, vinorelbine, and vinflunine) were extracted from the leaves of the Madagascar periwinkle Catharanthus roseus. They have been widely used in the management of both hematological and solid tumors. Current research has expanded the available compounds that bind to the vinca domain on the β-tubulin. These compounds include the halichondrins, which are isolated from the marine sponges. These compounds block mitotic progression and induce apoptosis in cancer cells. They are at various stages of clinical development for the treatments of multiple disciplines.
Isolated in the 1960s from the bark of a yew tree ( Taxus brevifolia ), paclitaxel has revolutionized the management of multiple oncologic disciplines (ie, ovarian, breast, lung bladder cancer, and prostate cancer). A semisynthetic analogue, docetaxel, was isolated from the needles of the European yew ( Taxus baccata ), and is equally as instrumental in the disciplines listed earlier. Novel formulations of taxanes engineered to circumvent common toxicities are in clinical practice. The epothilones and their analogues bind to the taxane site yet retain a unique mechanism of action. These agents are currently used in patients who are taxane refractory.
Historically, agents that bind to the colchicine site have not been targeted for anticancer development. However, recent interest has surfaced in the combretastatins, compounds isolated from the South African willow ( Combretum caffrum ). These agents bind to tubulin and show potent anticancer activity by inhibiting cell cycle progression inhibiting mitosis, thereby triggering apoptosis.
Collectively, these agents are referred to as modulators of microtubule dynamics and have been the mainstay in the treatment of both solid and hematological tumors for several decades.
Microtubule-targeting agents
Microtubule-targeting agents either inhibit microtubule polymerization, resulting in decreased microtubule polymer mass, or promote microtubule polymerization, resulting in increased microtubule polymer mass and stabilization. These compounds are characterized either as microtubule-stabilizing agents such as the taxanes and the epothilones or microtubule-destabilizing agents such as the vinca alkaloids and colchicines.
Microtubule-targeting agents bind to distinct binding sites on the β-tubulin. The vinca domain is located adjacent to the GTP binding site in the β-tubulin. The taxane site is located within the hydrophobic pocket between adjacent protofilaments in the lumen of the microtubule, whereas the colchicine site is located at the intradimer interface between the α- and β-tubulin.
The oldest classes of cytotoxic agents that interfere with microtubules are the vinca alkaloids. These agents (vincristine, vinblastine, vindesine, vinorelbine, and vinflunine) were extracted from the leaves of the Madagascar periwinkle Catharanthus roseus. They have been widely used in the management of both hematological and solid tumors. Current research has expanded the available compounds that bind to the vinca domain on the β-tubulin. These compounds include the halichondrins, which are isolated from the marine sponges. These compounds block mitotic progression and induce apoptosis in cancer cells. They are at various stages of clinical development for the treatments of multiple disciplines.
Isolated in the 1960s from the bark of a yew tree ( Taxus brevifolia ), paclitaxel has revolutionized the management of multiple oncologic disciplines (ie, ovarian, breast, lung bladder cancer, and prostate cancer). A semisynthetic analogue, docetaxel, was isolated from the needles of the European yew ( Taxus baccata ), and is equally as instrumental in the disciplines listed earlier. Novel formulations of taxanes engineered to circumvent common toxicities are in clinical practice. The epothilones and their analogues bind to the taxane site yet retain a unique mechanism of action. These agents are currently used in patients who are taxane refractory.
Historically, agents that bind to the colchicine site have not been targeted for anticancer development. However, recent interest has surfaced in the combretastatins, compounds isolated from the South African willow ( Combretum caffrum ). These agents bind to tubulin and show potent anticancer activity by inhibiting cell cycle progression inhibiting mitosis, thereby triggering apoptosis.
Collectively, these agents are referred to as modulators of microtubule dynamics and have been the mainstay in the treatment of both solid and hematological tumors for several decades.
Limitations in the clinical use of microtubule-targeting agents
Drug Resistance
Intrinsic or acquired drug resistance is a limiting factor in the clinical applicability of microtubule-targeting agents. Several mechanisms of tubulin-binding agent resistance have been described. One such mechanism is the result of deceased cellular drug accumulation caused by the overexpression of membrane-bound drug efflux proteins such as the P -glycoprotein. These proteins are a family of adenosine triphosphate (ATP)-dependent transporter proteins located in the cell membrane that are overexpressed in many tumors cell lines and effectively decrease the intracellular concentration of drug levels. Other mechanisms include direct alteration in tubulin-binding site and altered expression of tubulin isotypes (βI-tubulin, βIII-tubulin). Altered expression of tubulin isotypes has been reported to have an impact on microtubule dynamics, for example the expression of βIII-tubulin results in resistance to taxanes and vinorelbine. In addition to the mechanisms of resistance alterations in the levels mentioned earlier, intracellular location, posttranslational modifications, and function of microtubule-regulating proteins (tau, MAP2, MAP4) can influence the sensitivity to microtubule agents. High expression of tau has been associated with breast neoplasms that are less responsive to paclitaxel. Stathmin is a microtubule-sequestering protein that regulates the mitotic spindle by binding to tubulin heterodimers and inducing microtubule destabilization. Investigators have reported that overexpression of stathmin decreases breast cell sensitivity to paclitaxel and vinblastine. Changes to the microtubules induced by interactions with other cytoskeletal proteins are yet another mechanism of resistance. The human pregnane X receptor is known to be a master switch in drug resistance. Activation of this pathway leads to enhanced expression of cytochrome CYP3A4, which enhances metabolic degradation of drugs, resulting in drug resistance. This effect has been seen with epothilones as well as with taxanes.
Side Effect Profile of Microtubule-Targeted Agents
One significant hurdle in the use of taxanes is their poor solubility, necessitating the use of solvents as vehicles. For example, paclitaxel is highly insoluble in water and requires emulsification with solvents, such as polyoxyethylated castor oil (Cremophor EL) and ethanol to allow intravenous administration. These formulations have the potential to cause severe toxicities such as hypersensitivity reactions and sensory and motor neuropathy. In addition, Cremophor can entrap paclitaxel and result in reduced drug clearance and nonlinear pharmacokinetics.
Given the limitations of the current microtubule inhibitors, novel microtubule inhibitors are being investigated to circumvent resistance and toxicity and to deliver effective therapeutic choices.
Novel Microtubule-Targeted Agents
Novel taxanes
Novel formulations of paclitaxel have been introduced in to clinical care, including both ABI-007 (Abraxane), CT-2103 (Xytotax), and Cabazitaxel (Jevtana), which is a novel taxane characterized by decreased propensity for P -glycoprotein–mediated drug resistance.
ABI-007 (Abraxane) is an albumin-bound paclitaxel that is solvent free, reversibly binds paclitaxel, transports it across the endothelial cell, and concentrates in the vicinity of the neoplasm. This agent can be administered without the common predications. Preclinical data have suggested that this agent achieves higher antitumor activity and higher intracellular concentrations of active drug when compared with paclitaxel. ABI-007 was compared with polyethylated castor oil-based standard paclitaxel in patients with metastatic breast cancer. Patients (n = 454) were randomized to either ABI-007 260 mg/m 2 or paclitaxel 175 mg/m 2 . Significantly higher response rates and longer time to tumor progression were reported with ABI-007 (23.0 vs 16.9 weeks, respectively; hazard ratio [HR] = 0.75; P = .006). Grade 3 sensory neuropathy was more common in the ABI-007 arm than in the standard paclitaxel arm. No hypersensitivity reactions occurred with ABI-007 despite the absence of premedication and shorter administration time. A randomized phase II study compared ABI-007 administered triweekly and weekly with triweekly docetaxel as first-line treatment of metastatic breast cancer. A total of 302 patients were randomized to either 300 mg/m 2 of ABI-007 every 3 weeks, 100 mg/m 2 weekly for 3 of 4 weeks, 150 mg/m 2 weekly for 3 of 4 weeks, or docetaxel 100 mg/m 2 every 3 weeks. The investigators reported that ABI-007, regardless of dose, showed a greater overall response rate than docetaxel. This agent has been further explored in other disciplines such as gynecologic malignancies. Coleman and colleagues reported a phase II evaluation of ABI-007 in the treatment of recurrent or persistent platinum-resistant ovarian, fallopian tube, or primary peritoneal cancer. Eligible patients were defined by persistent or progressive disease after primary chemotherapy or recurrence within 6 months of treatment completion. Treatment consisted of ABI-007 100 mg/m 2 days 1, 8, and 15 on a 28-day schedule. Of the 47 evaluable patients, the investigators reported 1 complete and 10 partial responses (23%), whereas 17 patients (36%) had stable disease. The median progression-free survival (PFS) was 4.5 months (95% confidence interval [CI]: 2.2–6.7), whereas the overall survival (OS) was 17.4 months (95% CI: 13.2–20.8). Seventeen patients (36%) had PFS greater than 6 months.
CT-2103 (Xyotax) (paclitaxel poliglumex [PPX]), is a conjugate of α-poly- l -glutamic acid and paclitaxel. Like ABI-007, this macromolecular drug conjugate eliminates the need for Cremophor. PPX has been studied in recurrent or persistent ovarian or primary peritoneal cancer. In one phase II study, patients received PPX at 235 mg/m 2 every 21 days or 175 mg/m 2 . The investigators reported that 16% and 41% of patients had a partial response or experienced stable disease, respectively. The median PFS was 2.8 months (95% CI 1.48–4.8 months) and median OS was 15.4 months. The most frequent grade 3 or 4 toxicities were neutropenia, constitutional symptoms, gastrointestinal symptoms, and neuropathy. This agent is being explored as maintenance therapy in ovarian cancer (clinical trial GOG 212).
In a phase II study conducted by Lin and colleagues, an unexpected incidence of hypersensitivity reactions was noted with CT-2103 in patients with metastatic breast cancer. The investigators reported that CT-2103 had activity in this small study (response rate of 17%); however, neurotoxicity and hypersensitivity reactions were more frequent in this patient population than expected, and led to early termination of the trial. Grade 3 or 4 hypersensitivity reactions were observed in 4 patients; none occurred before cycle 4 of therapy. Given the delayed incidence of hypersensitivity reactions, it was suggested that these reactions were a true drug allergy, distinct from the hypersensitivity reactions seen with standard paclitaxel. Cabazitaxel (Jevtana) is a new taxane characterized by a favorable pharmacokinetic profile and a decreased propensity for P -glycoprotein–mediated drug resistance. In June 2010, it was approved for the management of metastatic hormone-resistant prostate cancer. The approval of cabazitaxel was based primarily on the TROPIC (Treatment of Hormone-Refractory Metastatic Prostate Cancer Previously Treated with a Taxotere-Containing Regimen) trial. De Bono and colleagues reported the results of a phase III trial in patients with metastatic castration-resistant prostate cancer who had received previous hormone therapy, but whose disease had progressed during or after treatment with a docetaxel-containing regimen. Patients received prednisone daily, and were randomly assigned to receive either 12 mg/m 2 mitoxantrone or 25 mg/m 2 cabazitaxel every 3 weeks. The primary end point was OS. Secondary end points included PFS and safety. The investigators reported that the median survival was 15.1 months (95% CI 14.1–16.3) in the cabazitaxel group and 12.7 months (11.6–13.7) in the mitoxantrone group. The HR for death of men treated with cabazitaxel compared with those taking mitoxantrone was 0.70 (95% CI 0.59–0.83, P< .0001). Median PFS was 2.8 months (95% CI 2.4–3.0) in the cabazitaxel group and 1.4 months (1.4–1.7) in the mitoxantrone group (HR 0.74, 0.64–0.86, P< .0001). The most common clinically significant grade 3 or higher adverse events were neutropenia, febrile neutropenia, and gastrointestinal events. This agent has provided a new avenue for patients with advanced prostate cancer.
The Epothilones
Epothilones are macrolide antibiotics that represent a unique class of antimicrotubule-targeting agents. Their mechanisms of action are similar to that of taxanes yet they show more potent activity and have the potential to evade the known mechanisms of taxane resistance, such as P -glycoprotein overexpression or the acquisition of mutations at β-tubulin-binding sites. Naturally occurring epothilones are classified as epoxides (A, B, E, and F) or olefins (C and D).
Epothilones A and B were isolated from the myxobacterium Sorangium cellulosum . The epothilones disrupt microtubule dynamics by binding to the β-tubulin subunit of the α-β-tubulin dimer. They stabilize microtubules and result in the induction of mitotic arrest and apoptosis. The binding site of epothilones overlaps with that of the taxanes on the β subunit of tubulin, but there is evidence that the 2 agents bind to tubulin differentially. The epothilones are more potent than both paclitaxel or docetaxel, with mean inhibitory concentration values in the nanomolar range.
Epothilones A and B show modest in vivo activity. Early use of these agents was hampered by metabolic instability and a narrow therapeutic window. To improve antitumor efficacy, epothilone analogues have been synthesized.
Patupilone EPO906
Patupilone is the unmodified product of epothilone B. Phase I studies have explored several schedules of administration and have suggested that unlike the other microtubule agents diarrhea is prevalent with this agent. Patupilone has been studied in several disciplines, including ovarian, colorectal, nonsmall lung cancer, gastric, prostate, and renal cell tumors. Chi and colleagues reported a phase II study of patupilone in patients with metastatic castration-resistant prostate cancer previously treated with docetaxel. Eighty-three patients were enrolled. A prostate-specific antigen (PSA) decline of 50% or greater occurred in 47% of patients. A partial response occurred in 24% of patients. Median time to PSA progression was 6.1 months (95% CI, 4.7–8.0) and median OS was 11.3 months (95% CI, 9.8–15.4). A phase I trial in patients with ovarian cancer (n = 45) reported an overall response rate of 19.5%, with a median duration of disease control of 15.8 months. This agent has also been studied in combination studies with carboplatin (area under curve, 5–6 every 3 weeks). The overall response rate was 62%, whereas 14% of patients achieved stable disease.
The phase II results have led to a randomized phase III trial comparing patupilone with pegylated liposomal doxorubicin (PLD). This recent phase III study (n = 829) included platinum-resistant and taxane-resistant patients with ovarian cancer and reported a significantly higher response rate than PLD (15.5 vs 7.9%), yet no OS benefit was appreciated (13.2 months for patupilone and 12.7 months for PLD).
One intriguing aspect of this agent lies in its ability to penetrate the central nervous system (CNS). In addition, patupilone is reported to have radiosensitizing properties. A recent phase I trial reported the combined therapeutic approach of concurrent cranial irradiation and patupilone (given every week and every 3 weeks) in patients with primary or secondary CNS malignancies. Primary CNS malignancies received radiotherapy (RT) to a median dose of 60 Gy. CNS metastases received whole-brain RT to a median dose of 37.4 Gy, and patients with recurrent gliomas underwent stereotactic RT to a median dose of 37.5 Gy. The investigators reported that when patupilone was combined with a variety of radiation doses and fractionation schedules, concurrent patupilone was well tolerated and safe, with a maximal tolerated dose of 8 mg/m 2 every 3 weeks.
Ixabepilone
Ixabepilone (BMS 247,550), a semisynthetic derivative of epothilone B, is the most widely investigated epothilone. In vitro studies have shown that the cytotoxicity of ixabepilone is 2.5 times that of paclitaxel. Several dosing schedules in phase I studies have led to the recommended phase II dose of 40 mg/m 2 . Common side effects reported in all studies included neutropenia, hepatic enzyme dysfunction, alopecia, and neuropathy and hypersensitivity reactions.
Ixabepilone was approved in 2007 by the US Food and Drug Administration for the treatment of metastatic breast cancer. Thomas and colleagues reported the results of 752 patients randomized to either ixabepilone 40 mg/m 2 plus capecitabine 2000 mg/m 2 on days 1 to 14 of a 21-day cycle, or capecitabine alone 2500 mg/m 2 . The primary end point was PFS. Ixabepilone plus capecitabine prolonged PFS relative to capecitabine (median, 5.8 vs 4.2 months; HR, 0.75; 95% CI, 0.64–0.88; P = .0003) and yielded increased objective response rates (ORRs) (35% vs 14%; P <.0001). Grade 3 to 4 treatment-related sensory neuropathy, fatigue, and neutropenia were more frequent with combination therapy, as was the rate of death as a result of toxicity with patients with liver dysfunction. The investigators concluded that ixabepilone plus capecitabine showed superior efficacy to capecitabine alone in patients with metastatic breast cancer pretreated or resistant to anthracyclines and resistant to taxanes.
Jassem and colleagues reported the results of a pooled analysis on a prespecified subset of patients whose disease relapsed within 12 months after adjuvant anthracyclines and taxanes. Patients received ixabepilone plus capecitabine (n = 149) or capecitabine alone (n = 144) as first-line chemotherapy for metastatic breast cancer. Analysis included PFS, OS, ORR, and toxicity. In 293 patients, ixabepilone plus capecitabine increased PFS (median: 5.6 months vs 2.8 months; HR, 0.58; P <.0001), overall response rate (46% vs 24%), and OS (median: 15.1 months vs 12.5 months; HR, 0.84; P = .208). Major toxicities of this regimen included neuropathy, neutropenia, and hand-foot syndrome.
The efficacy of ixabepilone has also been shown in other subsets, including patients with triple-negative disease. Perez and colleagues analyzed the efficacy and safety data of ixabepilone in women with triple-negative breast disease from several studies. Of 2261 patients evaluated in these trials, 556 (24.5%) had triple-negative tumors. In the neoadjuvant setting, ixabepilone produced a pathologic complete response rate in the breast of 26% in triple-negative patients (vs 15% in the nontriple-negative population). In patients with metastatic breast cancer, the overall response rates in the phase II ixabepilone monotherapy trials ranged from 6% to 55%, comparable with rates seen in patients with nontriple-negative tumors. The combination of ixabepilone and capecitabine in the phase II study resulted in an overall response rate of 23% in triple-negative patients. A similar overall response rate (31%) was observed for a preplanned pooled analysis of triple-negative patients in the phase III trials of ixabepilone plus capecitabine. The median PFS was significantly longer for triple-negative patients treated with ixabepilone plus capecitabine (4.2 months) compared with treatment with capecitabine alone (1.7 months). The overall consensus was that ixabepilone seems to offer an alternative chemotherapeutic agent for patients with triple-negative breast cancer.
Ixabepilone: Prostate Cancer
Despite the recent approval of docetaxel for the treatment of hormone-refractory prostate cancer, additional novel agents that can further improve patient outcomes are warranted. The epothilones have shown potent antitumor activity in vitro and in experimental animal models of prostate cancer. Studies of single-agent ixabepilone in patients with hormone-refractory prostate cancer have reported a confirmed PSA response rate. Rosenberg and colleagues recently reported a phase I study of ixabepilone, mitoxantrone, and prednisone in patients with metastatic castration-resistant prostate cancer previously treated with docetaxel-based therapy. Thirty-one percent of patients experienced PSA declines of 50% or greater, and 2 experienced objective responses. Of 21 patients treated with mitoxantrone 12 mg/m 2 plus ixabepilone 30 mg/m 2 or greater, 9 (43%) patients experienced PSA declines of 50% or greater (95% CI, 22%–66%).
Ixabepilone: Gynecologic Malignancies
A recent multi-institutional phase II trial of ixabepilone (20 mg/m 2 , days 1, 8, and 15 on a 28-day cycle) in platinum-resistant and taxane-resistant ovarian cancer has been reported. The overall response rate in 49 patients was 18.4%. Stable disease was the best response in 40.8% of the patients. The median PFS and OS were 4.4 and 14.8 months, respectively. These results are similar to other single-agent cytotoxics commonly used in this setting.
Dizon and colleagues conducted a phase II study to determine the response rate of ixabepilone in patients with persistent or recurrent endometrial cancer who had progressed despite standard therapy. Patients received ixabepilone 40 mg/m 2 as a 3-hour infusion on day 1 of a 21-day cycle. Fifty-two patients were entered on the study and 50 of these were eligible. The overall response rate was 12%; 1 patient achieved a complete remission (2%), and 5 achieved partial remission (10%). Stable disease for at least 8 weeks was noted in 30 patients (60%). The median PFS was 2.9 months, and the 6-month PFS was 20%. Major grade 3 toxicities were neutropenia, leukopenia, gastrointestinal, neurologic, constitutional, infection, and anemia. The investigators concluded that in a cohort of women with advanced or recurrent endometrial cancer who were previously treated with paclitaxel, ixabepilone showed modest activity of limited duration as a second-line agent.
Epothilone B analogue: sagopilone (ZK-EPO)
Sagopilone is a novel, fully synthetic epothilone currently being investigated. Morrow and colleagues reported the results of a phase II study in women with metastatic breast cancer. Patients received sagopilone 16 or 22 mg/m 2 as 3-hour intravenous infusion every 21 days. Among the 65 patients who were evaluable for efficacy, there were 3 confirmed responses, yet OS was not reached. The main treatment-related adverse events were sensory neuropathy and fatigue.
Studies have reported that sagopilone crosses the blood-brain barrier. Freedman and colleagues reported a phase II study of sagopilone (ZK 219,477; ZK-EPO) in patients with breast cancer with CNS metastasis. The primary end point was CNS ORR. Secondary end points included toxicity, PFS, and OS. Fifteen women, all of whom had progressive CNS disease despite whole-brain RT, were enrolled. Two patients achieved a partial response (ORR, 13.3%) and remained in the study for 6 cycles. Median PFS and OS were 1.4 months and 5.3 months, respectively. The most common grade 3 toxicities were lymphopenia and fatigue.
Epothilone D analogues: KOS-862 and KOS-1584
Two epothilone D agents, KOS-862, and KOS-1584, are undergoing clinical investigation. Konner and colleagues conducted a phase I trial to determine the maximum tolerated dose (MTD) of KOS-862. Thirty-two patients were enrolled. KOS-862 was well tolerated, with manageable toxicity, favorable pharmacologic profile, and the suggestion of clinical activity. Buzdar and colleagues conducted a phase II trial of KOS-862 in patients with metastatic breast cancer. Fourteen percent of women had a partial response; however, there was a high incidence of grade 3 neurotoxicity (18.5%). Lam and colleagues recently reported the results of a phase I study of KOS-1584 in patients with advanced solid tumors. Sixty-six patients were accrued. Diarrhea, arthralgias, and encephalopathy were dose-limiting toxicities. Two patients achieved partial responses, whereas 24 patients had stable disease. Further data on either agent are pending.
Microtubule-Destabilizing Agents
Vinca alkaloids
The vinca alkaloids are agents classified as destabilizing agents that cause microtubule polymerization, suppress treadmilling/dynamic instability, inhibit mitosis, and result in apoptosis. Vinca alkaloids have a well-established role both in solid and hematological malignancies. Vincristine is well established as a therapeutic agent in the treatment of leukemias, lymphomas, and sarcomas. Vinblastine is an integral agent in the management of patients with testicular cancer Hodgkin disease and lymphoma, whereas vinorelbine is used in the management of nonsmall cell lung cancer. Although vinorelbine was never approved for the management of patients with breast cancer, there is significant activity as a single agent as well as in combination with trastuzumab. Vindesine is being explored as a potential option in the management of acute lymphocytic leukemia.
Vinflunine
Vinflunine is a novel vinca alkaloid that destabilizes microtubules and decreases microtubule growth rate. Studies have reported a differential affinity for tubulin, a superior in vivo activity when compared with other vinca alkaloids, and a slow rate of resistance. This agent is water soluble, thereby obviating solvent vehicles.
Clinical studies have focused on transitional cell carcinoma of the genitourinary tract, nonsmall cell lung cancer, and mesothelioma. A dosing regimen of vinflunine of 280 to 350 mg/m 2 intravenously once every 21 days has been used in most trials. Neutropenia was the prominent toxicity observed in most studies. A phase II trial in breast cancer yielded encouraging results in that 18 of 60 patients experienced an objective response. This agent has also been combined with trastuzumab and has yielded responses: 8 of 17 patients experienced a partial response. The adverse side effects of this agent include neutropenia, fatigue, and constipation.
Halichondrin B analogue: eribulin mesylate
Eribulin mesylate is a microtubule-targeting chemotherapeutic agent that is a synthetic analogue of the natural compound halichondrin B. It was initially isolated from the sea sponge ( Halichondria okadai ). Eribulin targets microtubules and suppresses dynamic instability at microtubule positive ends through inhibition of microtubule growth, with little or no effect on shortening.
Eribulin binds at or near the vinca domain, a region that is located at the interface of 2 tubulin heterodimers. This agent has been investigated in several tumor types and is approved for patients with metastatic breast cancer. Cortes and colleagues recently reported the results of a phase III study (EMBRACE [Eribulin Monotherapy Versus Treatment of Physician’s Choice in Patients with Metastatic Breast Cancer]). Patients (n = 762) were randomly allocated to either eribulin mesylate (1.4 mg/m 2 ) or treatment of physician’s choice (TPC). Patients accrued to this study had received numerous previous lines of therapy. The investigators reported that OS was significantly improved in women assigned to eribulin (median 13.1 months, 95% CI, 11.8–14.3) compared with TPC (10.6 months, 9.3–12.5; HR, 0.81; 95% CI, 0.66–0.99; P = 0.041). The most common adverse events in both groups were asthenia or fatigue, and peripheral neuropathy.
Hensley and colleagues recently reported the activity of this eribulin mesylate agent in patients with ovarian cancer. Patients with recurrent, measurable epithelial ovarian cancer who had received 2 or fewer previous cytotoxic regimens were enrolled into 2 cohorts: platinum-resistant patients and platinum-sensitive patients. In the platinum-resistant cohort, 37 patients enrolled, and 36 patients were evaluable for response and toxicity. Two patients achieved a partial response (5.5%), and 16 patients (44%) had stable disease as their best response. The median PFS was 1.8 months (95% CI, 1.4–2.8 months). In the platinum-sensitive cohort, 37 patients were evaluable for response. Seven patients achieved a partial response (19%). The median PFS was 4.1 months (95% CI, 2.8–5.8 months). The major toxicity was grade 3 or 4 neutropenia (42% of platinum-resistant patients; 54% of platinum-sensitive patients).
Colchicines
Colchicine, isolated from the meadow saffron ( Colchicum autumnale ), is one of the earliest microtubule-targeting agents identified. As a microtubule-depolymerizing agent, it binds at the interface of the α- and β-tubulin heterodimers. Colchicine causes microtubule depolymerization by inhibiting lateral contacts between the protofilaments. Although colchicine has no clinical use in malignant disciplines, multiple agents that bind to the colchicines-binding site are undergoing investigation.
Combretastatin
Combretastatins were originally isolated Pettit and colleagues from the root bark of the Combretum caffrum tree have been shown to target the microtubule, inhibiting the polymerization of tubulin to microtubules. These agents show potent antineoplastic activity by inhibiting cell progression at mitosis and initiating apoptosis. Combretastatin A4 phosphate (CA4P) is a simple derivative of the natural product that was prepared to increase water solubility. CA4P has also been shown to be a vascular-disrupting agent. CA4P is in clinical trials for treatment of cervical, colorectal, nonsmall cell lung, prostate, ovarian, and thyroid cancers.
Panzem
Matei and colleagues studied the role of 2-methoxyestradiol (Panzem), a metabolite of estradiol that destabilizes microtubules and exerts antiangiogenic properties, in eligible patients with ovarian cancer. The primary end point was ORR. Eighteen patients were enrolled. The most common adverse events were fatigue, nausea, diarrhea, neuropathy, edema, and dyspnea (most being grade 1–2). There were no objective responses, but 7 patients had stable disease. Of those 7 patients, 2 patients had stable disease for greater than 12 months. The rate of clinical benefit was 31%. This agent has also been explored in neuroendocrine tumors and prostate cancer.
Maytansine analogues
Maytansine and its analogues (maytansinoids) are potent microtubule-targeted compounds that bind to tubulin at the vinca-binding site. Similar to vinca alkaloids, maytansine can depolymerize microtubules and arrest cells in mitosis. Maytansine shows greater cytotoxicity in cells than the vinca alkaloids; however, a limiting factor in the use of these agents is their narrow therapeutic window because of neurotoxicity and gastrointestinal effects. An attractive approach involving vectorization of microtubule-binding agents to the tumor cell using a monoclonal antibody has reintroduced these agents into clinical practice. Trials of trastuzumab-DM1 (T-DM1), a maytansinoid conjugated to the human epidermal growth factor receptor 2-specific therapeutic antibody trastuzumab, showed impressive efficacy in heavily pretreated patients with metastatic breast cancer. Phase I and phase II clinical trials of T-DM1 as a single agent and in combination with paclitaxel, docetaxel, and pertuzumab have shown clinical activity and a favorable safety profile in patients with HER2-positive metastatic breast cancer. Two randomized phase III trials of T-DM1 are recruiting patients: EMILIA (Open-Label Study of Trastuzumab Emtansine (T-DM1) vs Capecitabine+Lapatinib in Patients With HER2-Positive Locally Advanced or Metastatic Breast Cancer) is evaluating T-DM1 compared with lapatinib plus capecitabine, and MARIANNE (Study of Trastuzumab Emtansine [T-DM1] Plus Pertuzumab/Pertuzumab Placebo Versus Trastuzumab [Herceptin] Plus a Taxane in Patients With Metastatic Breast Cancer) is evaluating T-DM1 plus placebo versus T-DM1 plus pertuzumab versus trastuzumab plus a taxane.
Novel Targeted Agents
Given the clinical effectiveness of microtubule modulators in oncology, continued efforts to identify novel agents that target the mitotic spindle and regulate cellular progression through mitosis continue. Nontubulin (ie, the kinase inhibitors) are under investigation. Although the mechanisms involved are not straightforward, they may work in 1 of 3 possible mechanisms: (1) they result in prolonged mitotic arrest, signaling apoptosis, which is the mechanism of action of microtubule assembly inhibitors such as the taxanes and eribulin; (2) they may cause mitotic delays in metaphase, resulting in cell death; or (3) they cause a transient mitotic delay that causes inappropriate chromosomal segregation, which results in cell death after mitosis. Several are in clinical development, including aurora kinase (AK), pololike kinase (PLK), and kinesin spindle protein (KSP) inhibitors. The preliminary data on these agents are reviewed here.
AK inhibitors
Aurora A and B are serine/threonine kinases essential for the formation of normal mitotic spindles and function of centrosomes. Aurora A has been suggested to be an oncogene, but recent data suggest that although aurora A kinase amplification and overexpression are not sufficient to induce transformation, it creates the environment by which other cellular changes and genetic alterations occur to complete oncoplastic transformation. In addition to their roles in mitosis, aurora A and B are known to interact with other cellular processes important in oncogenesis, including those involving NF-κ-B, p53, and N-myc. They are also frequently overexpressed in human tumors and hence have been identified for further development in cancer treatment. Inhibition of AK has been shown to result in inappropriate chromosomal segregation, believed to be the result of effects on spindle assembly. Depletion of aurora A in vitro causes G2-M arrest, which results in apoptosis. Aurora B kinase plays an important role in mitosis and functions in both chromosome attachment and orientation. It is part of a chromosome passenger complex that includes inner centromere protein, borealin, and surviving.
Alisertib is an orally active AK inhibitor that preferentially inhibits aurora A kinase. It is a potent inhibitor of cell division in vitro and shows growth inhibition in tumor xenografts using both solid malignancy and lymphoma models. In 1 phase I trial, 61 patients were treated in 16 different cohorts evaluating daily dosing (7 days on/14 days off), divided dosing (4 times a day for 7 days followed by 14 days off), and divided dosing with the addition of methylphenidate or modafinil. Most patients treated were men with a median age of 60 years. The most common malignancies were colorectal, lung, genitourinary, and sarcoma. Seventy-nine percent had received 3 or more previous treatment regimens. The major dose-limiting toxicity (DLT) was neurocognitive changes and somnolence, which was grade 3 in 18%. It was otherwise well tolerated up to 60 mg/d in divided doses. Dose escalation was otherwise halted because of somnolence, which persisted despite psychostimulants. No responses were seen, but 9 patients had stable disease for at least 4 cycles. In a second phase I study of 43 patients, dose escalation using intermittent dosing in a 28-day cycle was conducted. The DLTs consisted of somnolence and transaminitis; however, it was deemed that treatment of 10 to 14 days of a 28-day cycle was feasible. MTD was established at 70 mg/d administered in 4 divided doses for 14 days of a 28-day cycle. Again, no clinical responses were observed.
MK-0457 was evaluated in a phase I study evaluating a 5-day continuous infusion schedule (doses 0.5–12 mg/m 2 /h were tested). A total of 16 patients participated in this trial and DLT (neutropenia) was observed at the 12 mg/m 2 /h dose level. Three of 16 patients had stable disease.
MLN8237 is another AK A inhibitor that is available orally. It underwent phase I testing as a once-daily dose administered 7 of 21 days, with doses ranging from 5 to 150 mg/d tested. The MTD was reached at 150 mg/d and consisted of neutropenia, mucositis, and somnolence. No responses were recorded, although 5 patients achieved disease stability. It continues in clinical trials as a single agent and with chemotherapy.
The selective AK B inhibitor barasetib (AZD1152) was evaluated at 2 different dosing schedules in advanced solid tumors in a European study that recruited 59 patients. MTD was set at 200 mg when used as a 2-hour infusion weekly and at 450 mg when dosed every 2 weeks. The DLT was the same in both schedules and consisted of neutropenia, which occurred in 58% of patients. Although no responses were recorded, 25% achieved stable disease. Another phase I to II study was performed in newly diagnosed or relapsed acute myelogenous leukemia (AML). The MTD determined in the phase I setting was 1200 mg, dosed as a continuous infusion for 7 days of a 21-day cycle. The overall hematologic response rate was 25%, with toxicity consisting of stomatitis as the primary DLT. The response rate was similar to that achieved in a Japanese phase I study in which a 19% response rate was noted in a population with advanced AML, although in this more advanced population the predominant toxicity was neutropenia.
Danusertib (PHA-739,358) is an intravenous pan-AK inhibitor that underwent phase I evaluation in solid tumors using a 24-hour infusion schedule every 14 days. Fifty-six patients were enrolled, with febrile neutropenia established as the DLT. The recommended phase II dose was established at 750 mg/m 2 , with granulocyte colony-stimulating factor recommended. Two responses were seen in this phase I study: a patient with lung cancer had an objective response that lasted for 23 weeks and a patient with recurrent ovarian cancer had a 27% reduction in tumor dimensions and a 30% decline in her cancer antigen 125. A second phase I study in Europe evaluated danusertib on a weekly schedule (3 weeks on/1 week off). Fifty-six patients underwent evaluation and, again, neutropenia proved to be dose-limiting. The MTD was established at 330 mg/m 2 when infused over 6 hours. Although no responses were recorded, 24% had stable disease and 5 patients remained progression free at 6 months. Danusertib continues in clinical evaluation, particularly in imatinib-resistant chronic myelogenous leukemia (CML) based on the finding that it inhibits the multidrug-resistant T315I mutant of Bcr-Abl, which is responsible for 25% or more of CML resistance to imatinib.
Other agents in this class include AS703569, SNS-314, and AMG-900. Early clinical trials are ongoing, with no results yet published.
PLK inhibitors
PLKs are serine/threonine kinases that are also involved in checkpoint regulation in mitosis. As with the AKs, they are highly upregulated in human malignancies. Depletion of PLKs in cancer cells results in decreased cell proliferation and viability by interruption of the spindle assembly, resulting in prolonged mitotic arrest and eventual apoptosis. A summary of published clinical trials involving this class is discussed.
GSK461364 is a competitive inhibitor of Plk-1. Forty patients were enrolled in a phase I study of this agent that evaluated 2 different schedules: 3 weeks on/1 week off and a semicontinuous 28-day cycle (days 1, 2, 8, 9, 15, and 16). The DLTs were grade 4 neutropenia, grade 3 to 4 thrombocytopenia, and thromboembolic events (which occurred in 20% of patients); MTD was established at 300 mg for weekly dosing and 225 mg for semicontinuous dosing. No responses were recorded. Fifteen percent achieved stable disease, including 4 patients with esophageal cancer. The investigators concluded that sufficient interest was seen, although they recommended prophylactic anticoagulation in subsequent studies.
BI 2536 is a small molecule Plk-1 inhibitor that underwent a phase I evaluation in patients with advanced solid tumors in which 25-mg to 250-mg doses were administered; patients showing clinical benefit were treated with additional courses. The MTD was set at 200 mg, with DLT defined as neutropenia (56% had grade 3–4 severity). No responses were recorded, although 23% treated at or above the MTD had stable disease for at least 3 months. A subsequent open-label phase I evaluation was performed in 70 patients, which tested 2 schedules: 2 weeks on/1 week off as a 1-hour infusion or as a 24-hour continuous infusion on day 1 of a 21-day cycle. The MTD with weekly dosing was established at 100 mg/dose. With the continuous infusion schedule, doses up to 225 mg were tolerated and an MTD was not reached. Both schedules were associated with significant neutropenia: grade 3 to 4 in 36% using weekly dosing and 50% with the 24-hour infusion. No responses were recorded; 32% had stable disease with weekly dosing.
An open-label randomized phase II study of BI 2536 was also conducted in patients with advanced nonsmall cell lung cancer. Ninety-five patients received BI 2536 as an intravenous infusion on day 1 (200 mg) or from days 1 to 3 (50–60 mg) of a 21-day cycle, with interpatient dose escalation allowed based on patient tolerance. There were 4 responses (overall response rate, 4.2%), and median PFS was 2 months. The median OS was 7 months and there were no differences in outcomes associated with drug schedule. Thirty-seven percent of patients had grade 4 neutropenia, and 2 drug-related deaths (sepsis and pulmonary hemorrhage) occurred.
ON 01,910.Na regulates mitotic pathways, including Plk-1. A first-in-man study involving 20 patients evaluated this agent as a 2-hour infusion on days 1, 4, 8, 11, 15, and 18 of a 28-day cycle. The MTD was established at 3120 mg/dose. The predominant toxicities were associated with skeletal and abdominal adverse events, as well as significant tumor pain. One objective response was recorded in a patient with recurrent ovarian cancer. It persisted for up to 24 months. A separate phase I study was performed in 13 patients with high-risk myelodysplastic syndrome. All patients were reported to have a response, including 4 who had a complete marrow response.
KSP inhibitors
Kinesins are enzymes that use ATP to translocate along or destabilize microtubules, and are important for the process of cell division. KSP is a specific kinesin expressed only in dividing cells and thus is critical to the organization of the mitotic spindle. Subsequent inhibition of KSP results in apoptosis because of mitotic arrest.
Ispinesib (SB-715,992) underwent phase II evaluation in 17 patients with metastatic or recurrent malignant melanoma. The dose and schedule used were 18 mg/m 2 as a 1-hour infusion on a 3-week cycle. Although no responses were observed, 35% had stable disease for a median of 3 months. Grade 3 adverse events were limited, but consisted of dizziness and blurry vision. Because of lack of activity, it was not recommended for further evaluation in this population.
MK-0371 is a C2-hydroxymethyl dihydropyrrole KSP inhibitor designed to circumvent P -glycoprotein efflux and optimized for antitumor properties by incorporation of fluorine. In phase I testing that involved 35 patients with taxane-refractory cancers, MT-0371 was evaluated using a 24-hour infusion schedule dosed every 21 days. The MTD was established at 17 mg/m 2 /d without evidence of myelosuppression. The DLT seen at higher doses consisted of prolonged grade 4 neutropenia. No responses were noted, but stable disease for at least 4 cycles was seen in 16 patients.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree